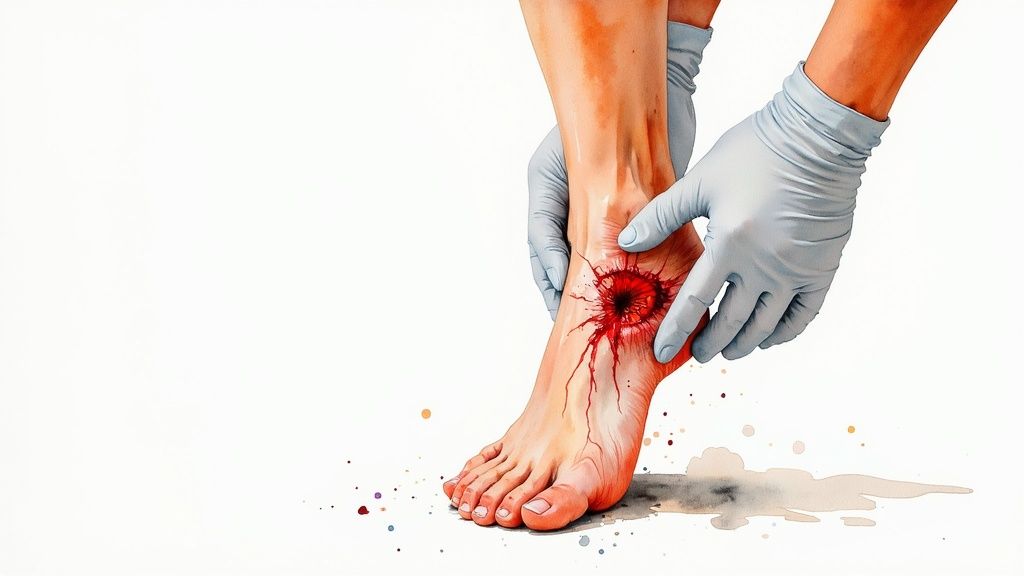
A wound care clinic is a specialized medical facility, but that description feels a bit sterile. It's really a dedicated center focused on one thing: healing wounds that have stubbornly refused to close on their own.
These aren't your everyday cuts and scrapes. We're talking about complex wounds like diabetic foot ulcers, persistent pressure sores, and surgical sites that just won't heal. Think of it as a high-level repair shop for the body, bringing in a team of experts who use advanced treatments to figure out what’s holding back your body's natural healing process.
The Role of a Specialized Healing Center

Here's a good way to think about it: if a wound is like a stalled car, your primary care doctor can give it a jump-start with basic first aid. But if the engine has a deeper, more complex problem, you need a master mechanic. A wound care clinic is that master mechanic for your body.
The entire focus is on answering one critical question: why isn't this healing? The answer is rarely simple. It could be poor circulation, an underlying condition like diabetes, or even a hidden infection that standard tests might miss.
To give you a clearer picture, here’s a quick overview of what a wound care clinic is all about.
Wound Care Clinic at a Glance
| Key Aspect | Description |
|---|---|
| Primary Focus | Treating chronic, non-healing wounds that resist conventional care. |
| Core Team | A multidisciplinary group including surgeons, podiatrists, and certified wound care nurses. |
| Common Conditions | Diabetic foot ulcers, venous ulcers, pressure injuries, and non-healing surgical wounds. |
| Key Approach | Diagnosing the root cause of healing delays, not just treating the surface symptoms. |
| Tools & Tech | Advanced diagnostics for blood flow and infection, plus therapies like debridement and skin substitutes. |
This table highlights how these clinics go far beyond the basics to provide truly specialized care.
More Than Just Bandages
A visit to a wound care clinic is completely different from a typical doctor's appointment where a wound might be one of several issues on the agenda. Here, the wound is the agenda. As key healthcare providers, these specialized centers are essential for patients with very specific needs.
They build a personalized roadmap to recovery that involves much more than just a new dressing. This often includes:
- A Collaborative Team: You'll find surgeons, podiatrists, infectious disease specialists, and certified wound care nurses all weighing in on your specific case.
- Advanced Diagnostics: They use tools to measure blood flow, pinpoint bacterial colonies, and assess tissue health in ways that simply aren't possible in a general practice.
- Targeted Therapies: Your treatment plan might include anything from debridement (the careful removal of unhealthy tissue) to bio-engineered skin substitutes or even hyperbaric oxygen therapy.
A wound care clinic bridges a critical gap in medicine. It provides focused, expert intervention when the body's natural healing process has been interrupted, preventing complications like severe infections and amputations.
By combining deep expertise with the right technology, these clinics create a dedicated path toward healing. They offer real hope and tangible results for wounds once considered incredibly difficult—or even impossible—to resolve, helping people get back on their feet and reclaim their quality of life.
When You Might Need a Wound Care Specialist
How can you tell when a cut is more than just a nuisance? Most scrapes heal just fine with a bandage and a little time. But some wounds are red flags, signaling a deeper problem that needs an expert’s touch. Knowing the difference is the first step in avoiding serious, long-term complications.
Think about a person with diabetes who finds a small sore on their foot. Instead of healing, it gets deeper. Or imagine an elderly patient who develops a pressure injury on their heel after being stuck in bed. Weeks go by, but the wound just won't close.
These situations are all too common. They represent the critical moment when a wound care clinic becomes absolutely essential. We specialize in managing wounds that get "stuck" and can't move through the body's natural healing process on their own.
Recognizing the Red Flags of a Non-Healing Wound
Any wound that doesn't show real improvement within two to four weeks is considered chronic. This is a major warning sign. Instead of getting smaller and less painful, a chronic wound might start showing some troubling symptoms.
Here are the key indicators that you need a specialist's help:
- No Progress After 30 Days: If a wound hasn't shrunk by at least 50% after four weeks of standard care, something is blocking the healing process.
- Worsening Pain or Odor: An increase in pain, redness, or swelling, or the development of a foul smell, often points to a bacterial infection that needs immediate attention.
- Excessive Drainage: While some fluid is normal, constant heavy drainage (exudate) can mean an infection or inflammation is preventing the wound from closing.
- Changes in Color: If the skin around the wound turns dark, black, or blue, it can signal a loss of blood flow—a condition called ischemia that requires urgent medical care.
If you see any of these signs, it’s time to go beyond basic first aid. Waiting can turn a manageable issue into a severe health crisis, potentially leading to widespread infection, a hospital stay, or even amputation.
Common Conditions Treated at a Wound Care Clinic
Wound care clinics are built to handle complex wounds, which are often tied to other health conditions. These underlying problems are usually the real reason a wound won't heal, as they can interfere with circulation, weaken the immune system, or disrupt the body's ability to repair itself.
For example, diabetic foot ulcers are one of the most common reasons patients come to us. High blood sugar damages nerves and reduces blood flow to the feet, meaning a tiny blister can become a serious, deep wound before the person even feels it.
The need for specialized wound care is a massive global health issue. An estimated 1.5 million Americans develop diabetic foot ulcers each year, and tens of millions worldwide suffer from chronic wounds, driving the demand for advanced treatments. You can explore more about the impact of chronic wounds from Spherical Insights & Consulting.
Other frequent cases we see include:
- Venous Stasis Ulcers: These typically appear on the lower legs and are caused by poor vein circulation, which leads to fluid buildup and skin breakdown.
- Pressure Injuries (Bedsores): These form from constant pressure on the skin, usually over bony areas like the hips, tailbone, or heels.
- Arterial Ulcers: Caused by poor blood flow in the arteries, these wounds are often very painful and can point to significant vascular disease.
- Non-Healing Surgical Wounds: Sometimes, an incision from surgery just doesn't close properly, leaving it open to infection and further breakdown.
In every case, the wound is just the symptom of a more complex problem. A wound care specialist’s job is to treat both the wound itself and the underlying issues preventing it from healing, creating a complete strategy for recovery.
Exploring Advanced Wound Healing Technologies
Walk into a modern wound care clinic, and you might feel like you’ve stepped onto the set of a sci-fi movie. The tools we use today are worlds away from simple bandages and ointments. Instead of just covering a wound and hoping for the best, clinicians now actively engineer the healing process at a cellular level, using specialized technology to break through the barriers that have stalled healing.

This isn't technology for its own sake; it delivers real, measurable results for the most stubborn wounds. By understanding these tools, you can see why a specialized clinic is uniquely equipped to succeed where other treatments have failed. Let’s pull back the curtain on some of the most powerful technologies used to restart the healing journey.
Hyperbaric Oxygen Therapy (HBOT)
Think of your body's healing cells as tiny construction workers trying to repair a damaged building. If they don’t have enough oxygen, they work slowly and get very little done. Hyperbaric Oxygen Therapy (HBOT) floods the worksite with the one thing they need most.
During an HBOT session, a patient relaxes inside a pressurized chamber while breathing 100% pure oxygen. This simple change allows the lungs to absorb far more oxygen than they ever could at normal air pressure. The bloodstream then carries this super-oxygenated blood throughout the body, saturating the wound site with the fuel it needs to build new tissue, fight off infection, and reduce swelling.
It’s like supercharging the body’s natural repair crew. HBOT is especially effective for wounds complicated by poor circulation, stubborn infections, or tissue damage from radiation.
Negative Pressure Wound Therapy (NPWT)
Another game-changer is Negative Pressure Wound Therapy (NPWT), which you might hear called a "wound vac." This device acts like a gentle, controlled vacuum, creating a perfectly sealed healing environment right over the wound.
A special foam dressing is placed inside the wound and covered with a clear film. A small tube connects this dressing to a portable pump that applies continuous, gentle suction. This clever process does several key things all at once:
- It pulls away excess fluid and harmful bacteria from the wound bed.
- It reduces swelling, which immediately improves blood flow to the area.
- It gently draws the wound edges together, encouraging them to close.
- It stimulates the growth of new, healthy granulation tissue.
NPWT is an excellent choice for large, complex, or heavily draining wounds because it creates a clean, moist, and controlled space for healing to happen.
Cellular and Tissue-Based Products
For wounds that cover a large area or have lost a significant amount of tissue, the body sometimes needs more than just a push—it needs a blueprint to rebuild upon. This is where Cellular and Tissue-Based Products (CTPs), often called bio-engineered skin substitutes, come into play.
These advanced products, derived from sources like donated human tissue, provide a structural scaffold that encourages a patient's own cells to move in and start rebuilding. They act like a temporary "skin," protecting the delicate wound bed while delivering the growth factors and proteins essential for new tissue to form.
CTPs are like laying down a fresh layer of fertile soil on barren ground. They provide the necessary structure and nutrients for new growth to take root, transforming a non-healing wound into an active site of tissue repair.
This approach is incredibly effective for diabetic foot ulcers, venous leg ulcers, and other chronic wounds that have hit a wall with conventional treatments.
Advanced Diagnostics: Seeing the Unseen
One of the biggest frustrations in wound care is battling an invisible enemy: bacteria. An infection can simmer just below the surface, completely stopping the healing process without any obvious signs. Modern clinics now use advanced diagnostic tools to "see" what the naked eye can’t.
One of the most impressive tools is fluorescence imaging, like the MolecuLight DX™ device. This handheld tool shines a safe, violet light onto the wound. In response, different types of bacteria glow in distinct colors, instantly revealing their precise location and concentration. This lets a clinician:
- Immediately detect high bacterial loads that are delaying healing.
- Guide debridement with incredible precision, removing only affected tissue.
- Target samples for lab testing far more accurately.
By making bacteria visible, clinicians can treat infections more effectively and build a cleaner foundation for healing. You can learn more about how this technology works with a point-of-care wound imaging device that detects the presence and location of elevated bacteria, which is transforming how specialists manage wounds. Treatment becomes targeted, efficient, and based on what’s actually happening inside the wound.
Meet Your Wound Care Team
Let's be honest: effective wound care is never a one-person job. It’s a team sport. Healing a complex wound is a lot like solving a puzzle with tons of interconnected pieces, and looking at it from just one angle is a recipe for failure. A true wound care clinic pulls together a multidisciplinary group of experts who all collaborate under one roof, with each person contributing a unique skill set to see the complete picture of your health.
This coordinated approach is what makes these clinics so powerful. Instead of you having to bounce between separate appointments with different specialists all over town, the team works together from the start. This structure avoids fragmented care and ensures that every single aspect of your wound—from blood flow to infection risk—is being addressed by a true expert.
The Core Players in Your Healing Journey
The real strength of a wound care clinic lies in this collaborative model. Clinical outcomes data has shown time and again that concentrating specialists like wound care nurses, podiatrists, and vascular surgeons is the key to successfully managing tough cases like diabetic foot ulcers. The entire model is designed to handle wounds with high morbidity and cost by bringing the right expertise together in one place. You can learn more about the market drivers for these specialized centers and see how workforce considerations impact clinic structure.
While the exact lineup can vary, your team will almost certainly include several of these key players:
- Wound Care Physician or Surgeon: Think of this person as the team's strategic leader. They diagnose the underlying reason the wound isn't healing, create the overall treatment plan, and perform advanced procedures like surgical debridement.
- Certified Wound Care Nurse: As the hands-on expert, this nurse is your go-to for day-to-day care. They'll be the one cleaning and dressing the wound, monitoring your progress, and giving you crucial education on how to manage your wound at home.
- Podiatrist: For any wound on the feet and ankles, especially those related to diabetes, a podiatrist is absolutely essential. They are experts in the unique biomechanics of the lower extremities and handle everything from offloading pressure to addressing foot deformities that get in the way of healing.
- Vascular Specialist: Blood flow is the supply line for healing—it brings all the good stuff (like oxygen and nutrients) to the wound. A vascular specialist assesses circulation to the area and can step in to restore blood flow if blockages in your arteries or veins are stopping the healing process in its tracks.
How the Team Works in Harmony
Let’s walk through a common scenario: a patient with a diabetic foot ulcer. The podiatrist immediately gets to work on the wound itself and any structural foot issues. At the same time, the vascular specialist is running tests to make sure enough oxygen-rich blood is actually reaching the foot to fuel tissue repair.
Meanwhile, the wound care nurse is executing the daily treatment plan, applying advanced dressings, and educating the patient on managing their blood sugar. Overseeing it all is the wound care physician, who adjusts the overall strategy based on the team's collective feedback and how the wound is progressing. This synergy is central to understanding what a wound care clinic really offers.
The power of a multidisciplinary team is that they treat the whole patient, not just the hole in the patient. By combining their expertise, they can address the root causes of why a wound is "stuck," leading to faster, more sustainable healing.
This integrated system is just far more effective than isolated efforts. Each professional provides a critical piece of the puzzle, and together, they build a comprehensive roadmap to get you back on your feet. For a deeper look into the specialists involved, you can get to know the different types of providers who form these expert teams and better understand their unique roles.
Navigating Your Path to Healing
Let's be honest, walking into any new medical facility can be a little intimidating, especially when you're dealing with a wound that just won't heal. But at a specialized wound care clinic, the entire process is designed to replace that anxiety with confidence. It all starts with getting to know you and your wound on a much deeper level.
Your first consultation is far more than just a quick look at the problem. It's a deep dive into your unique health story. The clinical team will review your full medical history, talk about your lifestyle, and learn what treatments you've already tried. This context is absolutely critical for figuring out why your healing process has stalled.
The First Step: Your Initial Assessment
This first visit is where the real detective work begins. The team’s primary goal is to uncover the root cause of the healing delay, which is often hiding beneath the surface. To get the full picture, they’ll use a combination of hands-on examination and advanced diagnostic tools.
This thorough assessment is what really separates a wound care clinic from a general practice. It typically involves:
- Wound Measurement and Staging: Carefully documenting the wound's precise size, depth, and other key characteristics.
- Vascular Assessment: Checking the blood flow to make sure the area is getting enough oxygen and nutrients to rebuild tissue.
- Tissue Analysis: Examining the wound bed itself for any signs of unhealthy tissue or a hidden infection.
This comprehensive evaluation builds the foundation for your entire treatment plan. It ensures that the team isn't just treating the visible wound, but also tackling the underlying issues that are preventing it from closing.
Creating Your Personalized Treatment Plan
Once the assessment is complete, the team works together to map out your personalized path to healing. This is never a one-size-fits-all situation. Your plan is built specifically around your type of wound, your overall health, and the realities of your daily life.
The team will walk you through every recommendation, explaining the "why" behind each proposed therapy. Your input is vital here—the plan is developed with you, not just handed to you. This collaborative approach makes sure the treatment is not only effective but also manageable for you.
The chart below shows how the different members of the wound care team work in concert to support your healing journey.
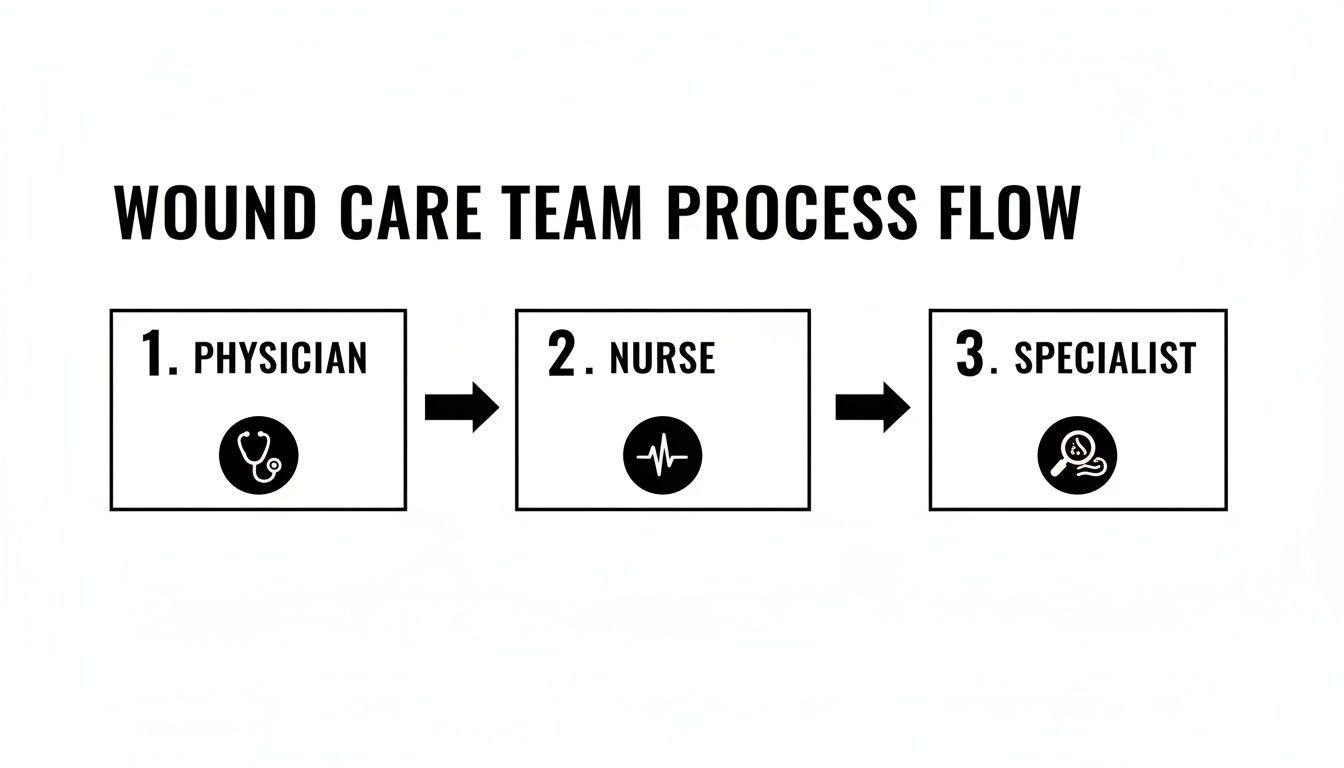
As you can see, the physician, nurse, and specialist all have interconnected roles, highlighting the coordinated care that is so central to getting a great outcome.
Regular Visits and At-Home Care
Your journey doesn't stop after the first visit. You’ll have regular follow-up appointments, often weekly. During these check-ins, the team will carefully clean the wound, perform necessary treatments like debridement (the removal of unhealthy tissue), and apply fresh, clean dressings. More importantly, they will meticulously track your progress, measuring the wound and documenting every sign of improvement.
But your role in this process is just as important as theirs. The team will give you clear, easy-to-follow instructions for at-home care, including how to change dressings, protect the wound from further injury, and manage your overall health to support healing.
Your active participation is a key driver of success. By following at-home care instructions and communicating openly with your team, you become a central partner in your own healing process.
As your wound gets better, your treatment plan will be adjusted to match. It's a dynamic approach that ensures you always receive the most appropriate care for where you are in the healing process. The ultimate goal is simple: to guide you, step-by-step, toward complete healing so you can get back to your daily life.
How to Choose the Right Wound Care Clinic
Let's be honest: not all wound care clinics are created equal. Finding the right one is a critical decision, whether you're a patient desperate for relief or a healthcare provider looking for a reliable partner for your patients. A great clinic does more than just throw technology at a problem; it delivers patient-centered, results-driven care that looks at the whole person, not just the wound on their body.
Making an informed choice comes down to knowing what to look for and which questions to ask. A top-tier clinic should be completely open about its approach, the expertise of its team, and its healing outcomes. This is how you find a center that is truly invested in getting the best possible results.
So, what exactly is a wound care clinic? Think of it as a specialized outpatient facility designed to treat complex wounds that just haven't responded to standard treatments. As healthcare has gradually shifted away from long inpatient stays, these focused centers have become essential. In fact, there are now an estimated 2,200 specialty wound care clinics in the United States, with most of them connected to hospitals. You can learn more about this growth from Towards Healthcare.
Key Questions for Patients and Families
When you or someone you love needs specialized care, you have to feel confident in your choice. Before you commit to a clinic, get on the phone or go in person and ask these questions to see if they're the right fit.
- What are your healing outcomes for wounds like mine? Any reputable clinic should be able to share data on their success rates for specific wounds, like diabetic foot ulcers or venous leg ulcers.
- How will you coordinate with my other doctors? Effective wound care is always a team effort. The clinic needs to have a clear process for communicating with your primary care physician, podiatrist, or other specialists involved in your health.
- What advanced technologies do you use? Ask them directly if they offer services like rapid diagnostics for bacteria, cellular tissue products, or even hyperbaric oxygen therapy.
- Who will be on my care team? You'll want to know about the credentials of the physicians and nurses. Look for special certifications in wound care and a team made up of experts from different disciplines.
These questions help you cut through the marketing fluff and get to the heart of a clinic's commitment to evidence-based, collaborative care.
Differentiators for Healthcare Professionals
If you’re a referring physician, case manager, or part of a home health agency, choosing a wound care partner is about more than just healing rates. You need a clinic that acts as a seamless extension of the care you already provide.
A top-tier wound care partner is defined by a commitment to clear communication, evidence-based practices, and a shared goal of reducing hospital readmissions. This alignment ensures continuity of care and better outcomes for shared patients.
Look for a partner that truly shines in these areas:
- Evidence-Informed Protocols: The clinic must follow proven best practices and use treatments backed by solid clinical evidence. This ensures your patients get the most effective care available.
- Robust Communication: A great partner gives you timely updates, sends detailed progress notes, and has an open line for direct communication. You should always be in the loop.
- Focus on Patient Education: The best clinics empower patients with the knowledge and tools they need to manage their care at home. This is huge for preventing complications and supporting long-term healing.
When you're looking for a clinic, it's also helpful to see how they make themselves available to the community. A proactive clinic will often employ smart local SEO strategies for medical practices to make sure they are visible and accessible online to the very patients who need their help the most.
Your Top Questions About Wound Care Clinics, Answered
Walking into a specialized medical environment like a wound care clinic for the first time can feel a little intimidating. It's natural to have questions. Getting clear answers is the first step toward feeling confident and in control of your healing journey.
Here are some straightforward answers to the questions we hear most often from patients and their families.
How Long Will My Wound Take to Heal?
This is usually the very first thing people want to know, and the honest answer is: it’s different for everyone. The time it takes for a wound to heal really depends on the type of wound, its size, your overall health, and how closely you can follow the care plan at home.
While there’s no magic number, the entire purpose of a specialized clinic is to drastically speed things up. We do this by figuring out why the wound stalled in the first place and targeting that root cause. Your team will give you a realistic timeline based on your specific situation and keep you updated on your progress every step of the way.
Is the Treatment Painful?
Your comfort is our priority. We know you’re already dealing with the daily pain of a chronic wound, and our goal is to not add to it.
Most of our advanced therapies are minimally invasive. For procedures that are absolutely necessary, like debridement (removing unhealthy tissue to let healthy tissue grow), our clinicians are experts in managing discomfort. We use local anesthetics and specific techniques to keep you as comfortable as possible. The most important thing is to speak up—if you’re feeling pain, tell us so we can adjust.
A key difference with a specialized clinic is the focus on a holistic patient experience. This means managing pain is considered just as crucial as the physical treatment of the wound itself, ensuring a more positive and sustainable healing journey.
Do I Need a Referral from My Doctor?
Navigating insurance can feel like a maze, but you’re not on your own. Some insurance plans do require a referral from your primary care doctor to see a specialist, but many others don't.
The administrative team at a wound care clinic lives and breathes this stuff. They’ll look into your specific insurance plan, let you know exactly what’s needed, and help you get any authorizations required. The goal is to get you the care you need without any frustrating delays.
For a deeper dive, you can explore more topics in our list of frequently asked questions about wound care.
How Is This Different from My Home Health Nurse?
Your home health nurse provides absolutely vital care, and we’re here to support their work, not replace it. It’s a partnership.
Think of it like this: your home health nurse is the expert on your day-to-day care and knows you best. The wound care clinic acts as a command center, bringing in advanced diagnostic tools and a team of different specialists who can all weigh in. This setup gives you the best of both worlds—consistent, compassionate care at home, supercharged by the technology and collaborative brainpower of a dedicated wound healing team.
At Specialty Wound Care, we combine advanced technology with expert clinical care to create personalized healing plans. Learn how our dedicated teams can help you or your patients move past a non-healing wound by visiting us at https://specialtywoundcare.com.