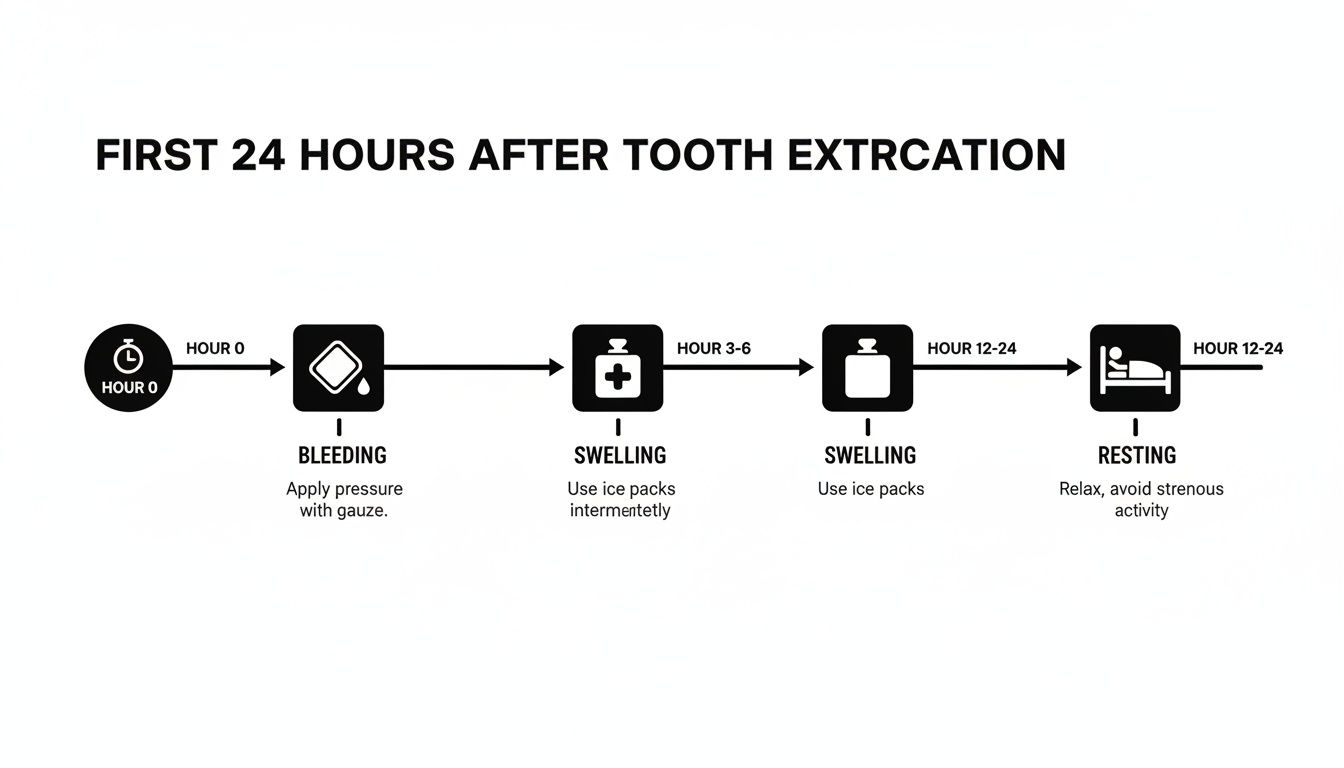
You've made it through the surgery, and now you're settling in at home. That first 24-hour window is, without a doubt, the most critical part of your recovery after wisdom teeth removal. What you do now directly impacts how the next week or so will play out.
Your body's main job is to form a stable blood clot in the empty tooth socket. Think of this clot as nature's own perfect bandage—it shields the underlying bone and nerves from everything. Protecting it is your number one priority.
Navigating The First 24 Hours
This isn't just a waiting game; it's an active healing phase where every little decision matters. Each year, about 5 million Americans have their wisdom teeth removed, and a typical recovery takes around two weeks. Swelling usually hits its peak on days two and three, and then the pain starts to ease up.
The key to staying on that timeline (or even shortening it) is to nail this first day. Let's walk through what you need to do, step by step. If you want a deeper dive, you can discover more insights about the post-extraction recovery period and what to expect.
Immediate Actions When You Arrive Home
The moment you get home, your recovery mission is officially on. You'll likely still be numb from the anesthesia, which is great—it gives you a head start to get comfortable before the discomfort creeps in.
The first thing to focus on is the gauze your surgeon placed. Bite down with firm, steady pressure. This isn't about soaking up blood; it's the pressure itself that stops the bleeding and helps that all-important clot form. Try not to talk too much or chew on the gauze, as any movement can disrupt things.
Key Takeaway: A little oozing mixed with saliva can look like a lot of blood, and that's totally normal. But if you find yourself soaking through bright red gauze pads every 30 minutes after a couple of hours, that's a sign to give your surgeon's office a call.
Once you’re settled, get an ice pack going. Wrap it in a towel (never apply ice directly to your skin) and place it on your cheek over the surgical area. The magic formula is 20 minutes on, 20 minutes off. This simple cycle is your best weapon against swelling. Starting immediately helps constrict the blood vessels and minimizes inflammation before it has a chance to really set in.
This timeline gives you a quick visual breakdown of your priorities for the day.
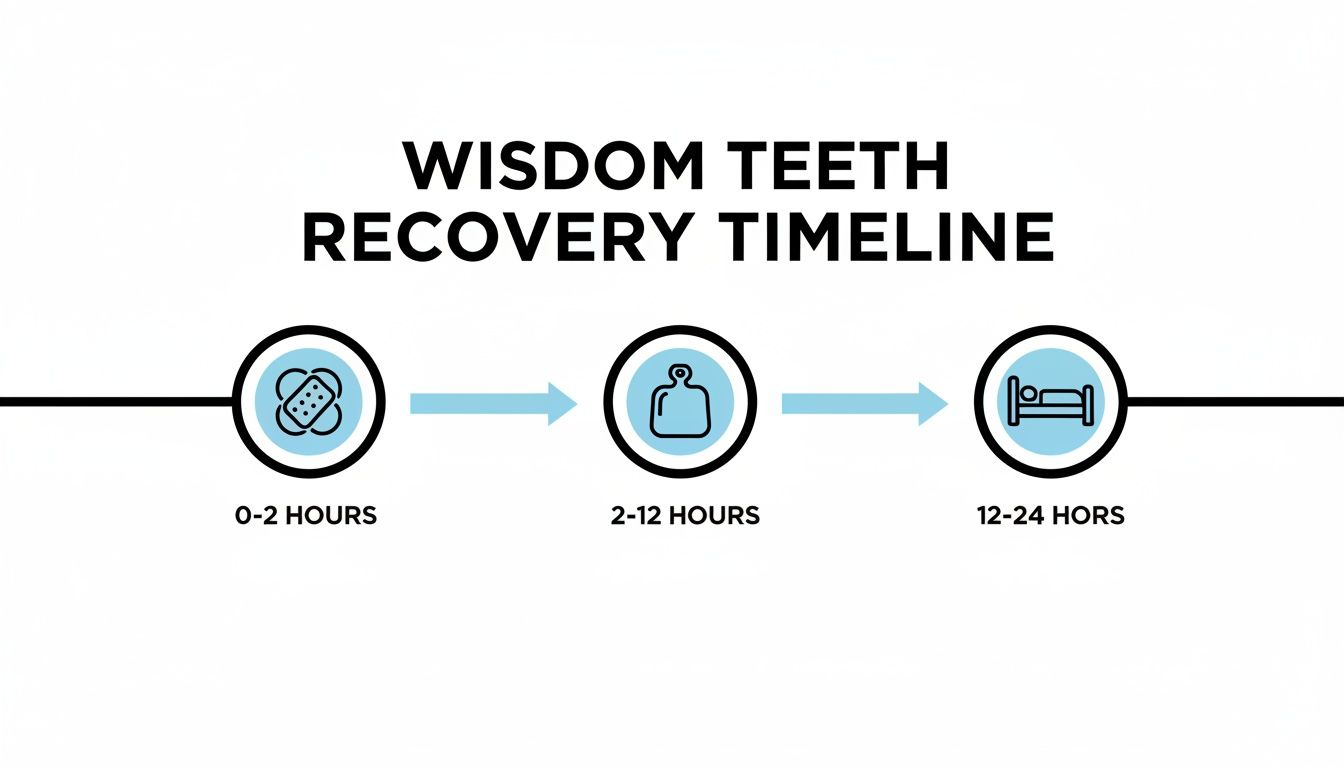
As you can see, the focus shifts from actively managing bleeding early on to controlling swelling and then prioritizing rest as the hours go by.
To help you keep track, here's a simple checklist of the do's and don'ts for this critical first day.
Immediate Post-Op Care Checklist (First 24 Hours)
This table summarizes the essential actions to take and things to avoid to protect the surgical site and manage your initial symptoms.
| Action/Symptom | What to Do | What to Avoid |
|---|---|---|
| Bleeding | Bite down firmly on gauze for 30-45 minutes at a time. | Chewing on gauze, excessive talking, spitting. |
| Swelling | Apply ice packs to the outside of your cheek (20 mins on, 20 mins off). | Applying heat, lying flat for long periods. |
| Pain | Take your first dose of pain medication before the anesthesia wears off. Stay ahead of the pain. | Waiting until the pain is severe to take medication. |
| Hydration/Diet | Drink plenty of cool liquids. Stick to soft, cool foods like yogurt, applesauce, or pudding. | Using straws, drinking hot liquids, eating crunchy or hard foods. |
| Rest | Lie down with your head elevated on 2-3 pillows. Rest and avoid any physical activity. | Bending over, strenuous activity, lying completely flat. |
Following these guidelines closely gives your body the best possible start for a smooth and speedy healing process.
Protecting The Surgical Site Is Everything
Nearly everything you do on day one circles back to protecting that blood clot. If it gets dislodged, you can end up with a dry socket, which is a notoriously painful complication you definitely want to steer clear of.
Here are the non-negotiable rules for the first week:
- No Spitting. The force from spitting can easily pull the clot right out of the socket. If you need to rinse, just let the liquid gently fall out of your mouth into the sink.
- No Straws. The suction creates a vacuum in your mouth, and it's one of the top causes of a dislodged clot.
- No Smoking. Beyond the chemicals interfering with healing, the physical act of inhaling can dislodge the clot.
- No Hot Liquids. Heat can dissolve the clot and may increase bleeding. Stick with cool or lukewarm options for now.
When it's time to rest or sleep, your position matters. Prop your head up with a couple of extra pillows to keep it elevated above your heart. This simple trick helps reduce swelling and minimizes that throbbing feeling. Lying flat allows blood to pool in your head, which increases pressure and discomfort. You'll be surprised at what a difference this small adjustment makes when you wake up the next morning.
A Realistic Plan For Pain And Swelling

Let's be honest: you're going to have some discomfort and swelling after your wisdom teeth are removed. It’s an unavoidable part of the process. But while you can’t skip it, you can absolutely get a handle on it with a smart, proactive approach.
The real goal here isn't to chase the pain after it starts, but to stay ahead of it. If you wait until you're already in serious discomfort, you're forced to play catch-up, and that's a tough battle. A well-timed strategy from the very beginning will make a massive difference in your recovery.
Building Your Medication Schedule
Your surgeon will likely prescribe a pain reliever and suggest an over-the-counter anti-inflammatory like ibuprofen. These two medications are a powerful team because they work differently. The trick is to create a staggered schedule.
For instance, you might take your prescription medication, and then three hours later, take the recommended dose of ibuprofen. Three hours after that, it's time for your next prescription dose. By alternating them, you maintain a consistent level of pain relief, avoiding those awful peaks and valleys of discomfort.
Pro Tip: Set alarms on your phone for your medication schedule, especially for the first 48-72 hours. It's surprisingly easy to lose track of time when you're resting, and those alarms are your best friend for staying ahead of the pain curve.
This method often helps you manage pain so effectively that you end up needing less of the stronger prescription medication overall. Just be sure to follow the dosage instructions from your surgeon and pharmacist to the letter.
Mastering Temperature Therapy
Temperature therapy is probably the best non-medical tool you have for managing symptoms, but it’s a two-part game. Using the wrong temperature at the wrong time can actually set you back.
The First 72 Hours: Ice Is Your Ally
For the first two or three days, your main mission is to fight inflammation. Cold therapy is how you win.
- How it Works: An ice pack constricts the blood vessels in your cheek. This reduces blood flow to the area, which minimizes swelling and helps numb the nerve endings for some welcome pain relief.
- The Method: Grab a gel pack or even a bag of frozen peas wrapped in a thin towel. Apply it to the outside of your jaw for 20 minutes, then take it off for at least 20 minutes.
- Why Breaks Are Crucial: Leaving ice on for too long can damage your skin tissue. That "off" period lets your skin return to a normal temperature before you apply the cold again.
Stick to this on-and-off cycle, and you'll stand a much better chance of avoiding those classic "chipmunk cheeks" that tend to show up on day two or three.
After 72 Hours: Switch to Warmth
Once you've passed the 72-hour mark, your goal changes. Now, you want to promote healing and ease up any muscle stiffness. It's time to bring in moist heat.
A warm compress, like a damp washcloth heated in the microwave (test it first!), helps increase blood circulation. This brings more oxygen and nutrients to the surgical sites to speed up the healing process. It also feels amazing on a stiff, sore jaw that’s been held open during surgery. For a deeper dive into managing jaw soreness, this guide to relief from jaw pain after wisdom teeth extraction offers more detailed strategies.
Finding a Comfortable Sleeping Position
How you sleep plays a huge role in swelling and comfort. Just like during the first 24 hours, keeping your head elevated is key for the first few nights.
When you lie flat, fluid can pool in your facial tissues, which increases pressure and that awful throbbing feeling at the extraction sites. Prop your head and upper body up on two or three pillows. This lets gravity work for you, helping to drain fluid away from your face. If you're a side sleeper, do your best to stay on your back for a few nights. If you can't, at least try to avoid putting direct pressure on the side where a tooth was removed.
What to Eat and How to Keep Your Mouth Clean
Figuring out what to eat and how to keep your mouth clean after wisdom teeth removal can feel like a huge challenge. Your mouth is sore, the surgical sites are incredibly delicate, and the last thing you want is to mess something up. The best way to approach this is in phases—start with the basics and slowly work your way back to your normal routine as you heal.
This isn't just about surviving on milkshakes for a week (though a little ice cream is definitely okay). It’s about giving your body the right fuel to heal while protecting those sensitive extraction sockets from getting irritated or infected. A smart plan here is just as critical as managing your pain and swelling.
Your Post-Surgery Eating Plan
For the first couple of days, your diet is going to be pretty limited, but it's essential for healing. The main goal is to eat foods that need zero chewing and won't disturb the fragile blood clots forming in the sockets. Think smooth, soft, and cool.
Right after surgery, you'll be sticking to liquids or puréed foods. This is all about staying hydrated and getting some easy calories in so your body has the energy it needs to start repairing itself.
Good Choices for the First 1-2 Days:
- Cool Soups: Smooth, blended soups like tomato or butternut squash are perfect. Just make sure they aren't hot.
- Smoothies: These are a great way to pack in nutrients. Add some protein powder, yogurt, or soft fruits like bananas. Just remember—absolutely no straws. Sipping can dislodge the blood clot, so drink right from the cup.
- Yogurt and Pudding: These are recovery staples for a reason. They're soft, cool, and require no effort to eat.
- Applesauce: A simple and gentle option to get some nutrients in.
- Meal Replacement Shakes: These can be a lifesaver for making sure you’re getting balanced nutrition when you can't really "eat."
Once you hit day three or four, you’ll likely start feeling a bit better and can begin adding in foods that need just a little bit of chewing.
A Quick Note on Temperature: Hot foods and drinks can increase blood flow to the surgical sites, which might cause bleeding or knock a clot loose. Stick with cool or lukewarm options for at least the first 48 hours. It's a simple step that makes a big difference.
When you're ready, you can move on to more substantial foods. This is the point where you'll start to feel like you're eating a "real" meal again.
Soft Foods to Introduce Around Days 3-7:
- Scrambled Eggs
- Mashed Potatoes or Mashed Sweet Potatoes
- Oatmeal or Cream of Wheat
- Soft, Flaky Fish (like Cod or Tilapia)
- Refried Beans
- Cottage Cheese
- Avocado
Foods and Habits to Absolutely Avoid
What you don't eat is just as crucial as what you do. The wrong foods can cause a lot of pain and lead to nasty complications like a dry socket or an infection.
For at least the first week, you need to avoid anything that could get stuck in the sockets or requires any real chewing effort. This means staying away from:
- Crunchy Foods: Chips, popcorn, nuts, and crackers.
- Hard Foods: Pretzels, hard candies, and tough cuts of meat.
- Chewy Foods: Gummy candies, steak, and crusty bread.
- Spicy or Acidic Foods: These will sting and severely irritate the healing tissue.
- Foods with Small Seeds or Grains: Things like strawberries, raspberries, quinoa, and sesame seeds are notorious for getting lodged in sockets and causing infections.
Keeping Your Mouth Clean Without Causing Harm
Good oral hygiene is non-negotiable for preventing infection, but your normal brushing routine is way too aggressive for the first few days. For the first 24 hours after surgery, you shouldn't do any rinsing, spitting, or brushing right near the surgical sites.
After that initial 24-hour window, you can start a very gentle cleaning routine. The idea is to keep things clean without disturbing the healing that’s already underway.
The Gentle Saltwater Rinse
Starting the day after your surgery, a warm saltwater rinse will be your best friend. It’s the most effective way to keep the sockets clean. Just mix half a teaspoon of salt into an eight-ounce glass of warm water.
- Take a small sip into your mouth.
- Gently tilt your head from side to side, letting the water flow over the surgical areas.
- Do not swish or spit forcefully. This is critical.
- Simply let the water fall out of your mouth into the sink.
Do this after every meal and before heading to bed. It’ll help flush out any food particles without putting pressure on the clots.
Brushing and Flossing Carefully
You can, and should, start brushing your other teeth again the day after surgery. Use a very soft-bristled toothbrush and be extremely cautious as you get near the back of your mouth. For the first few days, avoid the extraction sites completely. You can also gently brush your tongue—it’ll help your mouth feel a whole lot fresher.
How To Spot And Prevent Complications
While almost everyone heals just fine after wisdom teeth removal, knowing what isn't normal can bring a ton of peace of mind. The goal here is to understand the difference between typical recovery aches and the early signs of a real problem.
This isn't about scaring you. It's about empowering you to act fast if something feels wrong, stopping a small issue from turning into a big one.
Your main job is to prevent two key issues: dry socket and infection. Both are pretty rare, but they can seriously slow down your healing and cause a lot of unnecessary pain. The good news? The same simple aftercare that helps you heal—like avoiding straws and keeping the area clean—is your best defense against them.

Recognizing The Signs Of A Dry Socket
"Dry socket" is the complication everyone seems to have heard of. Officially called alveolar osteitis, it happens when the blood clot that forms in the empty tooth socket gets knocked out or dissolves too early. This leaves the bone and sensitive nerves exposed to air, food, and everything else in your mouth.
You'll know the pain from a dry socket—it’s nothing like the dull ache of normal healing.
- Timing: The pain usually kicks in around three to five days after your surgery, often right when you were starting to feel better.
- Pain: The biggest giveaway is a severe, throbbing pain that doesn't just stay at the surgery site. It often radiates up toward your ear, temple, or eye on that side of your face.
- Taste and Smell: You might also have a nasty taste in your mouth or bad breath that even saltwater rinses can't touch.
- Appearance: A quick peek with a flashlight might reveal whitish bone at the bottom of the socket instead of the dark, reddish clot you should see.
If this sounds like what you're experiencing, don't just try to power through it. Call your oral surgeon right away. Treatment is usually simple—they'll clean the socket and place a medicated dressing over it—but it's the only way to get real relief.
How To Identify A Possible Infection
Infections are another potential curveball, though they're less common than dry sockets if you’re following your aftercare instructions. Your mouth is full of bacteria, and a surgical wound can be an easy target.
The signs of an infection can look a lot like normal healing at first, with one critical difference: they get worse, not better, after the third day.
Key Takeaway: Swelling and pain should be at their worst around day three, then start getting noticeably better each day. If your pain, swelling, or general feeling of being sick suddenly spikes on day four or five, that’s a red flag. Time to call your surgeon.
Other warning signs of an infection include:
- Yellow or white pus draining from the extraction site.
- A persistent fever or chills.
- Swelling that makes it hard to open your mouth or swallow.
To help you tell the difference, here’s a quick comparison of what you can generally expect versus what should make you pick up the phone.
Normal Healing vs. Potential Complication
| Symptom | Normal Healing (Days 3-7) | Potential Complication (Warning Sign) |
|---|---|---|
| Pain | Gradually decreases. Managed with prescribed or OTC pain relievers. | Becomes severe, throbbing, or radiates to the ear/eye after day 3. |
| Swelling | Peaks around day 3, then steadily goes down. | Worsens or reappears after day 4; feels hard or hot to the touch. |
| Drainage | Minimal, clear, or slightly blood-tinged oozing in the first 24 hours. | Yellow or white pus coming from the socket; foul taste or odor. |
| Fever | A low-grade fever (under 101°F / 38.3°C) is possible in the first 24-48 hours. | A new or persistent fever develops after day 3. |
This table is just a guide, and your surgeon's advice is always the final word. When in doubt, call them.
An oral surgery site is a complex wound, and sometimes an infected socket can behave like a chronic wound, needing rapid diagnostics to pick the right antibiotics. In these cases, technology is a huge help. You can learn more about how a point-of-care wound imaging device detects the presence and location of elevated bacterial loads, allowing clinicians to make faster, more accurate treatment decisions. This gets you the right care quickly and stops an infection in its tracks.
Never hesitate to contact your provider if you think you have an infection. A course of antibiotics usually clears things up fast, but catching it early is the key.
Knowing When To Call For Help

Let’s be honest, recovering from wisdom teeth removal can feel like a guessing game. Is this much pain normal? Shouldn't the bleeding have stopped by now? Knowing the difference between a typical healing process and a genuine problem is the key to a smooth, worry-free recovery.
Most of the time, things heal up just fine. But your body has ways of telling you when something’s wrong. The most important thing you can do is listen to it and never hesitate to get professional advice.
Red Flags That Require Immediate Attention
Some symptoms are not up for debate—they should never be ignored. If you experience any of the following, it’s time to pick up the phone and call your oral surgeon's office right away, even if it's after hours. Waiting can quickly turn a manageable issue into a serious complication.
- Uncontrolled Bleeding: Some oozing for the first day is expected. Heavy, bright red bleeding that doesn't slow down after applying firm gauze pressure for over an hour is not.
- Severe Pain Unresponsive to Medication: Your pain should be getting better after day three, not worse. If the pain suddenly intensifies or your prescribed medication isn't touching it, that’s a major red flag for a complication like a dry socket.
- Signs of an Allergic Reaction: Watch for a skin rash, hives, or any difficulty breathing after taking medication. These symptoms point to an allergic reaction and demand immediate medical attention.
For a broader perspective on what constitutes an urgent issue, this ultimate guide to dental emergencies is a helpful resource.
When Normal Healing Stalls
Sometimes, the healing process just stalls out. You might not have the urgent red flags we just talked about, but the socket just isn't closing properly. Maybe it stays tender for weeks, or you notice other signs that it's just not getting better. This is when the surgical site becomes a chronic wound.
This is where the situation crosses a line from standard dental aftercare into the realm of specialized wound medicine. A routine oral surgery site should heal predictably. When it doesn't, it starts to behave like any other complex wound on the body and needs a more advanced strategy to get it back on track.
An oral wound that fails to heal properly is more than just a dental issue—it’s a chronic wound that needs specialized care. If you've been dealing with a non-healing surgical site for weeks, it's time to consider a different approach.
The Role Of A Wound Care Specialist
If you’re stuck with a surgical site that has turned into a chronic problem, a wound care specialist can bring treatments to the table that go far beyond what a typical dental office provides. They look at the wound on a cellular level to figure out exactly why it’s stalled.
Advanced treatments can make all the difference in these stubborn cases. For instance, fluorescence imaging can be used to see bacterial colonies that are invisible to the naked eye, allowing for much more precise treatment. In other situations, amniotic allografts can provide a biological scaffold for your body’s own cells to build new, healthy tissue, essentially giving the healing process a fresh start. These therapies are designed specifically for complex wounds that haven't responded to standard care.
If your recovery has hit a wall and you're worried about a wound that just won't heal, seeking specialized help is the most proactive step you can take. You can explore your options and book a consult with a wound care expert to get a detailed assessment and a personalized treatment plan designed to finally get you over the finish line.
Common Questions About Wisdom Teeth Recovery
Even when you follow your post-op instructions to the letter, questions are bound to pop up. Knowing what to expect—and what’s not normal—can make all the difference in feeling confident during your recovery.
We’ve put together the most common questions we hear from patients. Think of this as your go-to guide for those middle-of-the-night worries, helping you tell the difference between a normal healing ache and a genuine red flag.
How Long Does The Pain Actually Last?
This is the big one, isn't it? For most people, the most significant pain hangs around for three to five days. It typically peaks right alongside the swelling, usually around the 48 to 72-hour mark after your surgery.
After that peak, you should notice a real shift. The sharp, intense pain starts fading into a more manageable, dull soreness. If you start feeling better and then suddenly get hit with a severe, throbbing pain a few days later, that's a major warning sign for dry socket. Don't just hope it goes away—call your surgeon.
When Can I Start Working Out Again?
I know it’s tough to press pause on your fitness routine, but it's absolutely essential for a smooth recovery. You need to avoid all strenuous activity for at least one full week. No exceptions.
Why? Anything that gets your heart rate and blood pressure up can trigger more bleeding, swelling, and throbbing pain at the surgical sites. Worse, it can dislodge the blood clots that are so critical for healing, setting you back significantly.
- Days 1-4: Your only job is to rest. That means no lifting, bending over, or any real exertion.
- Days 5-7: You can start introducing some very light activity, like a slow walk around the block. Pay close attention to your body. If you feel any throbbing in your jaw, stop immediately.
- After Day 7: Assuming your recovery is on track and complication-free, your surgeon will likely give you the green light to slowly ease back into your normal routine.
Expert Tip: Don't be a hero and rush back to the gym. Even if you're feeling pretty good, those sockets are still incredibly delicate. Trying to do too much too soon is one of the fastest ways to cause a setback.
What Are The Telltale Signs Of A Dry Socket?
Dry socket is the most common complication people worry about, and for good reason—it is intensely painful. The classic sign is a sudden blast of severe, throbbing pain that appears three to five days after surgery, often after you've already started to feel better.
This pain is different. It doesn't just stay in the socket; it often radiates up toward your ear, temple, or even your eye on that side of your face. You might also notice a foul taste in your mouth or bad breath that doesn't go away with gentle saltwater rinses. If you look in the mirror, the socket might look visibly empty, missing the dark blood clot that should be there.
If you suspect a dry socket, don't wait. Call your oral surgeon’s office right away to get it treated.
Is A Stiff And Sore Jaw Normal?
Yes, a stiff, sore, and hard-to-open jaw is completely normal. It’s a condition called trismus, and it’s caused by swelling in the jaw muscles after they were held open during the procedure.
The stiffness usually feels worst around day three and then slowly gets better over the next week. Once you’re past the 72-hour mark, you can start applying a warm, moist compress to the outside of your jaw. This will feel great and help those tight muscles relax.
Gently trying to open and close your mouth can also help restore your range of motion, but never force it to the point of pain. For more answers to common questions, check out our FAQs about wound care.
At Specialty Wound Care, we know that a clear, supported healing journey is essential. If you are struggling with a surgical wound that just isn't getting better, our advanced diagnostics and treatments are here to help. Find out how we can support your recovery by visiting https://specialtywoundcare.com.