Your Guide to Understanding and Treating an Abscess on Gum
An abscess on the gum is more than just a painful lump; it's a serious red flag. Think of it as your body's emergency containment system trying to wall off a rapidly growing bacterial infection. This painful, pus-filled pocket is a battle your body can't win on its own, and it demands immediate professional attention to stop the infection from spreading.
Understanding a Gum Abscess and Why It Demands Urgent Care
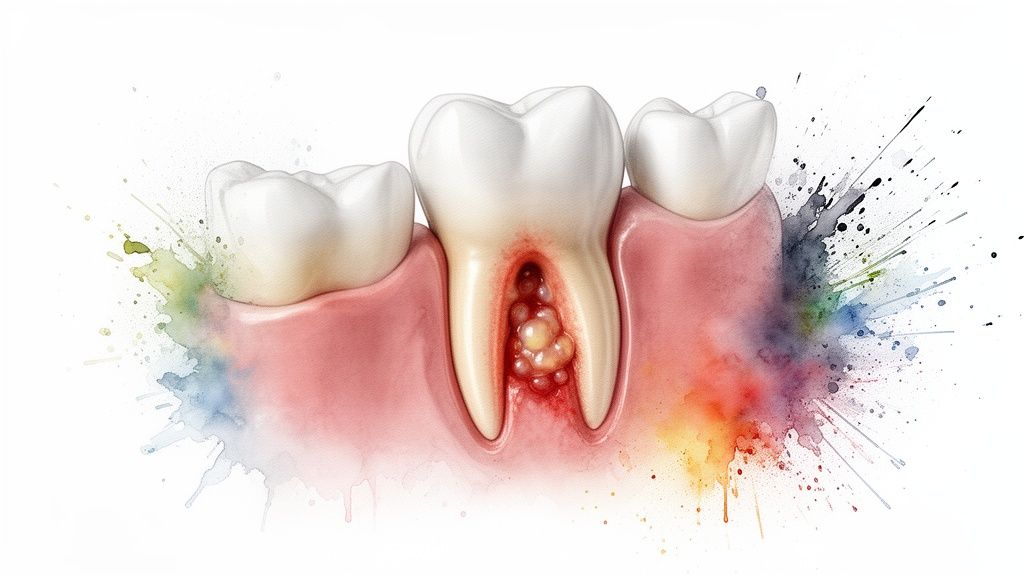
Picture a small but aggressive bacterial colony finding a weak spot deep in your gum tissue or at the root of a tooth. Your immune system immediately goes on the defense, sending white blood cells to fight off the invaders. This intense conflict creates a pocket filled with pus—a mix of dead bacteria, tissue, and immune cells—which we see and feel as a painful, swollen lump. That's a gum abscess.
Ignoring this warning sign is a dangerous gamble. If left untreated, the bacteria will multiply and spread. This can lead to tooth loss, damage to the jawbone, or even a systemic infection that travels through your bloodstream, affecting your entire body.
That’s why an abscess on the gum is a true dental emergency. Knowing the difference between a minor issue and a crisis is key, making understanding when to seek emergency dental care essential for your health and safety.
The Two Primary Types of Gum Abscesses
Not all abscesses are created equal. Where the infection starts—its origin story—determines the entire course of action. Pinpointing the source is the first critical step toward getting the right treatment.
Let's break down the two main types you might encounter.
Periodontal Abscess vs Periapical Abscess
The table below offers a quick comparison of the two main types of dental abscesses to better understand the potential source of the infection.
| Feature | Periodontal Abscess (Gum Origin) | Periapical Abscess (Tooth Origin) |
|---|---|---|
| Source | Infection starts in the gum pocket next to a tooth. | Infection begins inside the tooth's pulp (nerve). |
| Primary Cause | Advanced gum disease (periodontitis) traps bacteria. | Severe tooth decay, cracks, or trauma lets bacteria in. |
| Location | Swelling appears on the side of the gum, often near the gumline. | Swelling is typically at the tip of the tooth root, visible on the gum. |
| Associated Pain | Often a dull, continuous ache; may be sensitive to biting. | Usually a sharp, throbbing, severe pain that can be intense. |
| Tooth Vitality | The associated tooth is often still alive and healthy. | The associated tooth is usually non-vital (dead) or dying. |
Understanding this distinction is far more than just academic—it's the roadmap for treatment. A periodontal abscess often calls for deep cleaning and drainage, while a periapical abscess usually requires a root canal or tooth extraction to get to the source.
These infections are surprisingly common. Dental abscesses are behind a significant number of urgent care visits, making up about 8% of all emergency dental appointments worldwide. In the U.S. alone, severe dental infections result in around 200,000 emergency room visits annually. That’s a quarter of all oral health-related ER trips, a statistic that hammers home just how critical it is to recognize an abscess on the gum and seek professional help without delay.
Recognizing the Symptoms and Uncovering the Root Causes
A gum abscess doesn't just show up unannounced. It's the painful final act of a story that starts with a simple bacterial invasion. Figuring out how this happens—and what warning signs to watch for—is your first line of defense.
Think of your gum tissue as a fortress wall. When something creates a breach in that wall, it’s an open invitation for bacteria to storm in, set up camp, and multiply. Several common dental problems can tear down these defenses, essentially rolling out the red carpet for an infection.
Tracing the Infection Back to Its Source
The road to a full-blown gum abscess often begins with what seem like minor issues that slowly spiral out of control. Pinpointing the original culprit is absolutely critical. Why? Because just draining the abscess isn't a permanent fix; you have to solve the underlying problem, or it will just keep coming back.
Here are the usual suspects:
- Untreated Gum Disease: This is the big one. When plaque and tartar build up, they force the gums away from the teeth, creating deep pockets. These pockets are the perfect dark, damp hideouts for bacteria to get trapped and thrive.
- Deep Tooth Decay: A cavity that bores its way into the tooth's soft inner pulp—where the nerve lives—gives bacteria a direct route to the core. From there, the infection travels down the root and explodes into an abscess in the gum tissue right at the tip.
- Dental Trauma: A cracked, chipped, or broken tooth is like a broken window in your home's security. It creates a clear pathway for bacteria to invade the sensitive inner layers, sparking an infection that can quickly lead to an abscess.
- A Foreign Object Gets Stuck: Sometimes, it’s as simple as a tiny piece of a popcorn kernel getting wedged deep into the gum tissue. If it stays there, it irritates the area and triggers an infection, which can eventually form an abscess.
These conditions create the ideal breeding ground for bacteria to flourish, ending in a painful gum abscess. The scale of these underlying problems is staggering. Periodontal diseases are a massive global health burden, with an estimated 1.07 billion prevalent cases worldwide in 2021. In fact, over 42% of adults over 30 have some form of gum disease, which just goes to show how common these precursor conditions really are. You can find more details on the global impact of periodontal diseases on PMC.
Identifying the Telltale Warning Signs
While a visible, pimple-like bump on your gum is the most obvious giveaway, an abscess sends out plenty of other distress signals. Catching these early can get you to seek help before the infection digs in deeper. The pain, in particular, can be intense and hard to ignore.
An abscess often announces itself with a severe, persistent, throbbing pain. It can radiate from the tooth into your jaw, up to your ear, or down into your neck. This isn't just a minor ache that you can push through; it’s a constant, demanding pain telling you something is seriously wrong.
Keep a close eye out for these key symptoms:
- Intense, Persistent Pain: A throbbing ache that makes it hard to chew, focus, or even think straight.
- Extreme Sensitivity: A sharp, severe pain when anything hot or cold touches the tooth.
- Visible Swelling: You might see noticeable swelling in your gums, cheek, or the side of your face.
- Foul Taste or Bad Breath: If the abscess bursts, you might get a sudden rush of salty, foul-tasting fluid in your mouth. Persistent bad breath is another common sign.
- Systemic Symptoms: A fever, feeling generally unwell (malaise), and having tender, swollen lymph nodes under your jaw or in your neck are signs the infection is spreading.
These symptoms are your body’s fire alarm. They’re warning you that a localized infection is getting worse. While professional treatment is non-negotiable, you can find some relief from the severe discomfort. There are several helpful at-home soothing tips for dental abscess pain that can offer temporary comfort while you wait for your appointment. Just remember, these are stopgap measures, not a cure. They can't replace a visit to your dentist.
How Dentists Pinpoint the Cause of a Gum Abscess
When you show up at the dentist with a throbbing, swollen gum, it’s understandable to feel a bit on edge. But knowing how your dentist will get to the bottom of the problem can make the whole experience less stressful. Getting a precise diagnosis for an abscess on the gum is the critical first step, making sure the treatment hits the true source of the infection, not just the visible symptoms. Think of it as a methodical investigation to figure out exactly what’s going on under the surface.
It all starts with a conversation about what you're feeling and your overall health history. Then, your dentist will perform a gentle but thorough clinical exam. They're basically a detective looking for clues—inspecting your gums, teeth, and nearby tissue for any redness, swelling, or a draining fistula, which is a tiny tunnel the abscess forms to let out pus.
They'll also likely tap lightly on your teeth. This simple technique, called a percussion test, helps zero in on whether a specific tooth is the culprit. It's a quick way to help distinguish between an abscess starting in the gum (periodontal) and one originating from a tooth root (periapical).
Seeing Beneath the Surface with Dental Imaging
A visual check gives the dentist a lot of good information, but the real story of an abscess is often hidden deep inside a tooth or in the jawbone. To see what the naked eye can’t, your dentist will take dental X-rays. This is a non-negotiable step for getting the diagnosis right.
An X-ray serves as a blueprint of your mouth, showing exactly where the infection began and how far it has spread.
- Finding the Source: For a periapical abscess, the X-ray might reveal a dark spot right at the tip of a tooth’s root, a clear sign of infection that started in the tooth's nerve.
- Checking for Bone Loss: If it’s a periodontal abscess, the image can show bone loss around the tooth, a classic sign of advanced gum disease.
- Planning the Treatment: The details from the X-ray help your dentist decide on the best course of action, whether it's a root canal, a deep cleaning, or, in more serious situations, removing the tooth.
Without this step, any treatment would just be a temporary fix. It's like patching a leaky pipe but never shutting off the water—the problem is guaranteed to come back.
Advanced Diagnostics for Tricky Infections
For most gum abscesses, a good clinical exam and a clear X-ray are all that's needed to create a solid treatment plan. But what about infections that keep coming back? Or when a patient has a weakened immune system? Sometimes, an infection just doesn’t get better with the first round of treatment. In these cases, we need to dig deeper. The goal shifts from simply identifying the problem to understanding the specific germs causing all the trouble.
This is where rapid pathogen testing makes a huge difference. Instead of waiting days for traditional lab cultures to grow, this technology can quickly identify the exact bacteria fueling the infection. More importantly, it can tell us which antibiotics will actually work against them.
By identifying the specific pathogen, clinicians can move beyond broad-spectrum antibiotics and select a targeted medication. This precision approach not only improves treatment outcomes but also helps combat the growing problem of antibiotic resistance.
This level of detail is a major leap forward in oral healthcare. When your team knows precisely what they're up against, they can build a personalized and highly effective treatment plan from day one. You can learn more about this by exploring the benefits of advanced pathogen detection in wound care. This modern approach ensures a faster, more predictable recovery from a serious abscess on the gum.
Your Step-By-Step Gum Abscess Treatment Plan
Getting a gum abscess diagnosis can be alarming, but thankfully, the treatment path is well-defined. Tackling an abscess on the gum isn't a one-and-done fix. It’s a multi-stage process designed to give you immediate relief, knock out the infection, and fix the underlying issue so it doesn’t come roaring back.
Each step is critical. We start by handling the immediate pain, then shift to controlling the bacteria, and finally, resolve the root cause for good. This methodical approach is the key to a full recovery.
Stage 1: Immediate Relief Through Incision and Drainage
First things first: we need to relieve the intense pressure and pain from that trapped infection. We do this with a straightforward but incredibly effective procedure called incision and drainage (I&D). Your dentist makes a tiny, precise incision over the abscess, which allows all the built-up pus to drain out.
You'll feel an almost instant wave of relief as that pressure vanishes. It’s a crucial first step for managing pain and kicking off the healing process. Just remember, this only treats the symptom—the painful pocket of pus—not what caused it in the first place.
After draining, the area is cleaned thoroughly with a saline solution to wash away any lingering bacteria, calming the inflammation and setting the stage for what comes next.
Stage 2: Controlling the Infection with Antibiotics
With the pressure gone, the next job is to get the bacterial infection under control and prevent it from spreading. While drainage removes the bulk of the bacteria at the site, microscopic bugs can still be hiding in the surrounding tissues or even get into your bloodstream.
This is where antibiotics step in. Your dentist will likely prescribe a course of medication to fight the infection systematically from the inside out.
Think of antibiotics as essential backup. They help manage the infection throughout your body, but they can't fix the dental problem that let the abscess form.
It's absolutely vital to finish the entire course of antibiotics, even if you start feeling a lot better after just a day or two. Stopping early lets the toughest bacteria survive, setting you up for a recurring and more resistant infection down the road.
Stage 3: Addressing the Root Cause for a Lasting Cure
This is the most important part of the whole plan. Without fixing the original problem, the abscess is almost guaranteed to return. The specific treatment you’ll need depends entirely on whether it’s a periodontal (gum-based) or periapical (tooth-based) abscess.
Using your exam and X-rays, your dentist will pinpoint the best course of action.
- For a Periodontal Abscess: If the infection started in the gum pocket from advanced gum disease, the definitive treatment is a deep cleaning called scaling and root planing. This procedure gets rid of tartar and plaque below the gumline and smooths the tooth roots, helping the gums reattach and closing off the pockets where bacteria love to hide.
- For a Periapical Abscess: If the abscess came from an infection inside the tooth's nerve, a root canal treatment is the usual solution. This process removes the infected pulp, disinfects the inside of the tooth, and seals it up. In severe cases where the tooth is too damaged to save, an extraction might be necessary to remove the source of infection completely.
This flowchart shows the diagnostic path a dentist follows, from the initial look to the final tests that confirm the right treatment.
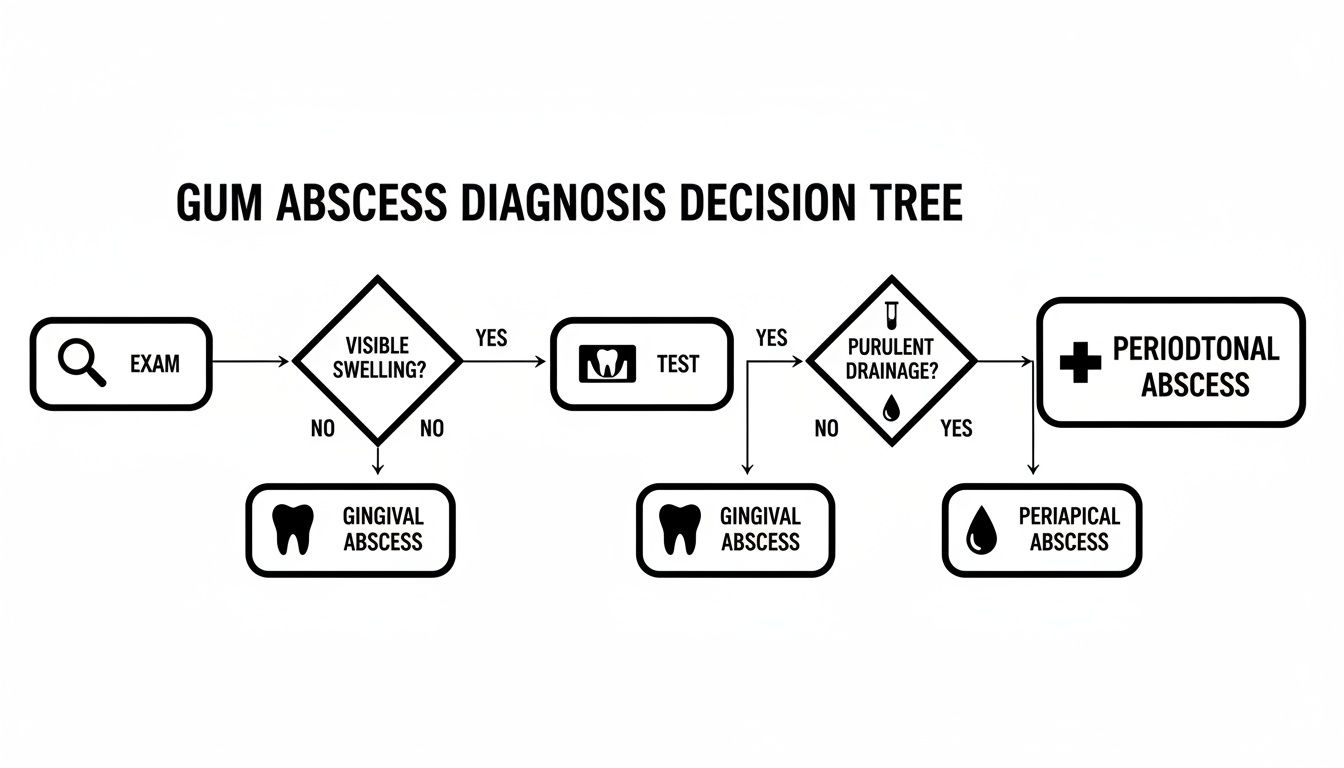
Each step in this visual guide builds on the last, ensuring the final treatment plan is precisely targeted to where the abscess started.
Stage 4: Post-Procedure Wound Management and Follow-Up
Once the main treatment is done, the ball is in your court. Proper wound care at home is essential for a smooth, quick recovery. Your dentist will give you specific instructions—make sure you follow them to the letter.
These instructions usually cover a few key areas:
- Maintaining Oral Hygiene: You'll need to keep the area clean, which often means gentle brushing and using a special antimicrobial rinse.
- Managing Discomfort: Over-the-counter pain relievers can help with any soreness after the procedure.
- Dietary Adjustments: Sticking to soft foods for a few days helps prevent irritating the healing tissue.
Finally, showing up for your follow-up appointments is non-negotiable. These visits let your dentist check on your healing, make sure the infection is totally gone, and confirm the underlying problem is solved for good, protecting you from another abscess on the gum.
Advanced Wound Care for a Faster Recovery
Healing from an abscess on the gum isn’t always a straight line, especially once the infection is drained. For some people, particularly those managing underlying health issues like diabetes or a weakened immune system, the site can turn into a complex wound that just won’t heal.
In these cases, standard home care simply isn't enough. This is where advanced wound care protocols come in. They aren’t just extra steps; they are targeted, proactive treatments designed to give your body the support it needs to truly regenerate damaged tissue.
When Healing Stalls and Standard Care Isn't Cutting It
For a healthy person, the small wound left after draining an abscess usually heals without much fuss. But when that healing process stalls—showing signs of stubborn inflammation, slow closure, or even reinfection—it’s a clear signal that the body needs more help. This is a common hurdle for patients whose systems are already working hard to manage other health challenges.
Think of it this way: standard care clears the debris from a construction site. Advanced care brings in the master builders and premium materials to reconstruct the building faster, stronger, and more resilient than before. These advanced methods are designed to break through the biological roadblocks that can turn a simple wound into a chronic problem.
One of the most effective tools in our kit is the use of biological scaffolds. For example, amniotic membrane allografts can be placed over the wound, acting as a natural framework. This scaffold is rich with the essential growth factors and proteins your body needs to build new, healthy gum tissue, giving a powerful jump-start to a stalled healing process.
Using Technology to Guide Treatment
A major challenge in managing a post-abscess wound is making sure it's truly clean. Even after drainage and a round of antibiotics, microscopic colonies of bacteria can stick around, creating what we call a high bacterial bioburden. This invisible threat is one of the main reasons some wounds just refuse to close.
To get ahead of this, modern wound care uses sophisticated imaging technology. Fluorescence imaging, for instance, allows a clinician to see the exact location and concentration of harmful bacteria on the wound’s surface in real-time. This isn’t guesswork; it’s a precise map showing exactly where to clean and debride the tissue. You can learn more about point-of-care wound imaging devices and how they guide treatment.
This table helps illustrate when it's time to transition from basic home care to a more specialized approach.
Standard Home Care vs Specialized Wound Management
A guide to understanding post-procedure care and when advanced wound management may be necessary for optimal healing.
| Care Task | Standard Home Care Instructions | Triggers for Specialized Wound Care |
|---|---|---|
| Cleaning | Gentle rinsing with warm salt water or a prescribed antimicrobial mouthwash. | Persistent pus drainage, a foul odor, or redness that spreads after initial treatment. |
| Monitoring | Watching for reduced swelling, less pain, and the gradual closing of the incision site. | Healing that has stalled for 7-14 days, or if symptoms are getting worse instead of better. |
| Follow-Up | A routine check-up to confirm the infection is gone and healing is on track. | Patients with diabetes, autoimmune disorders, or a known history of non-healing wounds. |
The ultimate goal of advanced wound care is to create the perfect environment for your body to heal itself. By removing barriers like high bacterial loads and providing regenerative support, we can significantly reduce recovery times and minimize the risk of the abscess returning.
By bringing in these advanced tools and strategies, we shift the focus from passively managing a wound to actively regenerating healthy tissue. This proactive approach helps patients recover more completely from an abscess on the gum, preventing long-term complications and restoring their oral health.
When a Gum Abscess Becomes a Medical Emergency
Most gum abscesses are urgent dental problems, but some cross the line into a full-blown medical emergency. This happens when the infection breaks free from its starting point in your mouth and begins to overwhelm your body’s defenses.
Recognizing the tipping point from a localized dental issue to a systemic threat is critical. An infection on the move can lead to sepsis, a life-threatening chain reaction where your body’s own immune response starts to damage its tissues and organs. Knowing what to look for isn’t just helpful—it can be a lifesaver.
Unmistakable Red Flag Symptoms
If you have a suspected gum abscess and notice any of the following signs, don't waste time calling the dentist. Get to an emergency room immediately for medical care.
-
Difficulty Breathing or Swallowing: This is the most alarming red flag. If swelling spreads to your throat or neck, it can start to close off your airway. Any trouble breathing or even swallowing your own saliva is a true medical emergency that needs immediate intervention.
-
High Fever and Facial Swelling: A fever is your body's normal response to an infection, but a high, stubborn fever (over 101°F or 38.3°C) paired with major swelling in your cheek, jaw, or down into your neck is a sign the infection is spreading aggressively.
-
Rapid Heart Rate and Confusion: Feeling dizzy, disoriented, or mentally foggy? Is your heart racing? These are classic signs that the infection may have entered your bloodstream, putting you at risk for sepsis. This requires urgent hospital care.
These symptoms mean the bacteria are no longer contained. They've breached the local defenses in your mouth and are starting to impact your entire system.
Preventing Future Gum Abscesses
The old saying holds true: an ounce of prevention is worth a pound of cure. The best way to sidestep a dental emergency is with consistent, proactive oral care. This is your number one defense against the problems that lead to abscesses in the first place.
Prevention is all about consistency. When you disrupt the bacterial colonies that cause decay and gum disease, you’re essentially knocking down the foundation an abscess needs to form.
Here are the most effective steps you can take to guard your oral health:
- Impeccable Oral Hygiene: It’s non-negotiable. Brush twice a day with fluoride toothpaste and floss at least once daily. This clears out the plaque and food debris that get stuck between teeth and under the gumline, where trouble starts.
- Regular Dental Visits: Don't skip your six-month check-ups and cleanings. Your dentist is trained to catch the earliest signs of decay or gum disease long before they have a chance to blow up into a painful infection.
- Mindful Diet: Sugar is fuel for the bacteria that cause cavities. Limiting sugary foods and drinks starves them out. A balanced diet doesn't just help your teeth; it supports your overall health, too.
Remember, untreated tooth decay is a wide-open door for infection. Oral diseases are incredibly common, affecting nearly 3.7 billion people worldwide, with untreated dental cavities being the single most common health condition. By tackling dental issues head-on, you dramatically reduce your risk of ever developing a painful—and potentially dangerous—abscess. You can discover more insights about global oral health on MedlinePlus.
Common Questions About Gum Abscesses
When you’re dealing with a gum abscess, it’s natural to have a few questions. Let's walk through some of the most common concerns to give you clarity and confidence on what to do next.
Can a Gum Abscess Heal on Its Own?
Absolutely not. A gum abscess will never resolve by itself. The pain might fade for a little while if it happens to burst and drain, but that’s misleading. The real source of the infection is still active deep inside the tissue.
Without professional treatment to clear out the pus and fix the root cause—whether it’s gum disease or a dying tooth—the infection will linger. It’s almost guaranteed to come back, and worse, it can spread into your jawbone or even your bloodstream, creating a much more serious health risk.
How Can I Manage the Pain Before My Dental Visit?
While you're waiting for your appointment, there are a couple of things you can do to manage the discomfort. Gently rinsing your mouth with warm salt water a few times a day is a great first step. It helps soothe the inflammation and can even draw out some of the infection.
Over-the-counter pain medications like ibuprofen can also be a big help, as they work to reduce both the pain and the swelling.
Remember, these are just temporary fixes to help you get by. They are no substitute for the professional care you need to eliminate the infection for good.
Is a Root Canal or Tooth Extraction Always Necessary?
Not always. The right treatment is all about pinpointing where the infection started. Your dentist’s diagnosis is the key to figuring out the best plan of action.
- Periapical Abscess: If the infection began inside the tooth’s nerve, then yes, a root canal or an extraction is usually necessary to get rid of the source.
- Periodontal Abscess: If the infection is from gum disease and started in the pocket between your tooth and gum, it can often be treated with a thorough deep cleaning procedure.
For more answers to common questions about dental and wound care, you can find a wealth of information by reviewing our comprehensive list of frequently asked questions.
At Specialty Wound Care, we are dedicated to resolving complex wounds with advanced diagnostics and treatments. If you are struggling with a non-healing oral wound or any persistent infection, we provide the specialized care needed for a full recovery. Learn more at https://specialtywoundcare.com.
