Amniotic Membrane Wound Healing: Innovative Therapy for Chronic Wounds
For a chronic wound that just won't heal, like a stubborn diabetic foot ulcer, the situation can feel hopeless. Week after week, standard treatments might fail, leaving the wound stuck in a frustrating and dangerous cycle of inflammation. This is an all-too-common reality where the body’s own healing mechanisms have essentially given up.
Amniotic membrane wound healing offers a powerful way to break that cycle. It’s a therapy that uses nature's own design to give the body the powerful boost it needs to get back on track.
The Power of Amniotic Membranes in Modern Wound Care
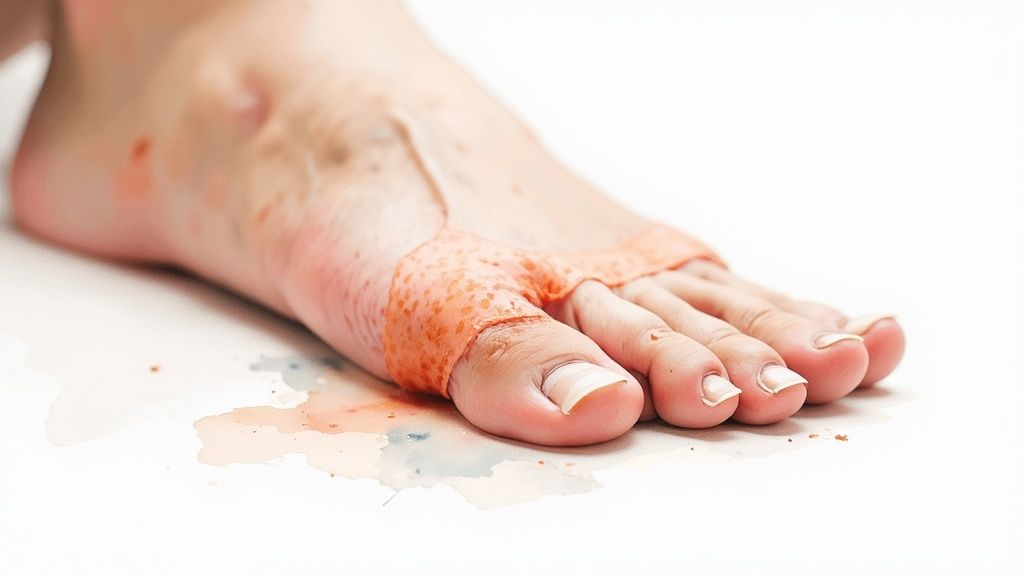
An amniotic membrane allograft is much more than a simple bandage. This is a sophisticated, biological tissue taken from the innermost layer of the placenta. Think of it as a complete wound-healing toolkit, packed with all the essential elements needed to build new, healthy tissue.
It’s an incredible resource that helps us address the root causes of a stalled wound, not just the symptoms.
A Natural Blueprint for Repair
When we apply an amniotic membrane to a chronic wound, it works on multiple levels. First, it provides a natural scaffold—a physical structure that new cells can latch onto and grow across. But its real power lies in the rich biological cocktail it contains.
This material is brimming with a unique combination of components that get to work immediately:
- Growth Factors: These are the "foremen" of tissue repair. They are powerful signaling molecules that tell the body’s cells to start multiplying, moving into the wound bed, and forming new tissue.
- Anti-inflammatory Proteins: Chronic inflammation is a major roadblock to healing. These proteins help calm this persistent inflammation, creating a much better environment for the repair process to finally begin.
- Anti-scarring Properties: Instead of allowing the body to form weak, disorganized scar tissue, the membrane helps guide the formation of healthy, functional skin.
By delivering this complete healing package directly to the wound, an amniotic membrane allograft essentially reawakens the body's own regenerative engine. It provides both the building blocks and the instruction manual that the wound has been desperately missing.
From Historical Discovery to Modern Therapy
Using this remarkable tissue isn't a new idea. In fact, the history of amniotic membrane in healing goes back more than a century to 1910, when Dr. John S. Davis first documented its successful use in skin grafting.
What's changed is the science behind its preservation. Modern processing techniques now allow us to safely preserve these grafts for years, making them readily available as an "off-the-shelf" advanced therapy. If you're interested in the deep dive, you can read more about the history and development of amniotic membrane usage in the National Library of Medicine.
This journey from a century-old discovery to a modern-day staple sets the stage for its powerful applications today.
How Amniotic Membranes Orchestrate Healing
To really get a handle on how powerful amniotic membranes are, it helps to think of a chronic wound as a construction site that’s completely stalled out. The crew has walked off, the blueprints are gone, and the whole project is stuck in a state of chaos. An amniotic membrane allograft is like a new project manager showing up with a skilled crew, a clear set of instructions, and all the high-quality materials needed to get the job done right.
This incredible biological material kickstarts healing through four key actions that all work together. They create the perfect environment for the body to start rebuilding tissue, finally breaking the cycle of inflammation that keeps a wound from closing.
A Natural Scaffold for New Growth
First things first, the amniotic membrane provides a physical structure. It’s made of a rich Extracellular Matrix (ECM), which is basically a natural, biological scaffold. Imagine trying to build a new wall without any framework to hold it up—it’s just not going to happen. New cells trying to repair a wound face the same exact problem.
The ECM in the amniotic membrane gives these cells something to grab onto. It provides a lattice they can use to crawl across the wound bed, get organized, and start the hard work of rebuilding. This structural support is the foundation for everything else that follows.
Think of the ECM as the foundational framework of a new building. It provides the essential structure that allows other specialized components—like growth factors and new cells—to come in and do their jobs effectively and in an organized manner.
The Power of Cellular Communication
On top of its structure, the amniotic membrane is loaded with a powerful cocktail of growth factors. These are essentially signaling proteins that act like traffic directors for cells. In a chronic wound, all the normal communication between cells has broken down. Growth factors get that conversation started again with clear, direct commands.
They send out signals that tell cells to perform specific jobs that are absolutely essential for healing:
- Proliferation: Telling local cells to multiply, creating the workforce needed for the repair job.
- Migration: Guiding these new cells to move into the wound bed where they are needed most.
- Differentiation: Instructing cells to become the specific types of tissue required, like new skin or blood vessels.
This targeted communication jumpstarts a healing process that had previously gone silent. It’s one of the main reasons we see such great results with amniotic membrane wound healing in stalled wounds.
Calming the Fires of Inflammation
Chronic inflammation is the main villain in the story of a non-healing wound. It’s like a fire that just won't go out at the construction site, constantly damaging materials and stopping any real progress. Amniotic membranes contain powerful anti-inflammatory agents that act like peacekeepers, effectively putting that fire out.
These agents work by telling the body to dial down the pro-inflammatory signals that fuel the destructive cycle. By calming the wound environment, the membrane creates a space where regenerative processes can finally take over. Making this shift is absolutely critical to move a wound from a chronic state onto a healing path. Some advanced products, like a dual-layer allograft, are specifically designed to maximize the delivery of these essential components.
Promoting Functional Tissue Regeneration
Finally, the membrane is brilliant at preventing excessive or disorganized scarring. Instead of letting the body form weak, non-functional scar tissue, it guides the growth of tissue that is much more like the original, healthy skin.
It does this through its unique mix of growth factors and matrix proteins, which encourage organized collagen to form. The result is a repair that is not only closed but also more durable and functional. These anti-scarring properties help ensure the newly formed tissue is strong and resilient, which lowers the risk of the wound breaking down again in the future.
These four healing mechanisms are the pillars of what makes amniotic membranes so effective. When they work in concert, they provide a comprehensive solution to the complex problems that keep a chronic wound from healing.
Below is a quick summary of how these pillars work together to drive the healing process forward.
Key Healing Mechanisms of Amniotic Membranes
| Mechanism | Biological Function | Impact on Wound Healing |
|---|---|---|
| ECM Scaffold | Provides a structural framework made of collagen and other proteins. | Enables new cells to migrate and attach, bridging the wound gap. |
| Growth Factors | Act as signaling molecules that direct cellular activity. | Stimulate cell multiplication and guide the formation of new tissue. |
| Anti-Inflammatory | Contain proteins that reduce chronic inflammatory responses. | Calms the wound, creating a stable environment conducive to repair. |
| Anti-Scarring | Modulate fibroblast activity and collagen organization. | Promotes the growth of healthy, functional tissue instead of weak scar tissue. |
By addressing the wound on multiple fronts—providing structure, directing cellular traffic, reducing inflammation, and preventing scarring—amniotic membranes give the body the tools it needs to overcome barriers and achieve complete, durable healing.
Clinical Applications and Proven Outcomes
Knowing the science behind amniotic membrane allografts is one thing, but seeing them work in a real clinic is what truly matters. This isn't just a fascinating biological concept; it's a practical tool we use to tackle some of the most stubborn wounds out there. The graft’s unique blend of a natural scaffold, growth factors, and anti-inflammatory agents gives us a way to address the specific biological roadblocks that keep chronic wounds from healing.
The power of these allografts really comes down to three core pillars working together.
This diagram breaks down the three pillars that make these grafts so effective in practice.
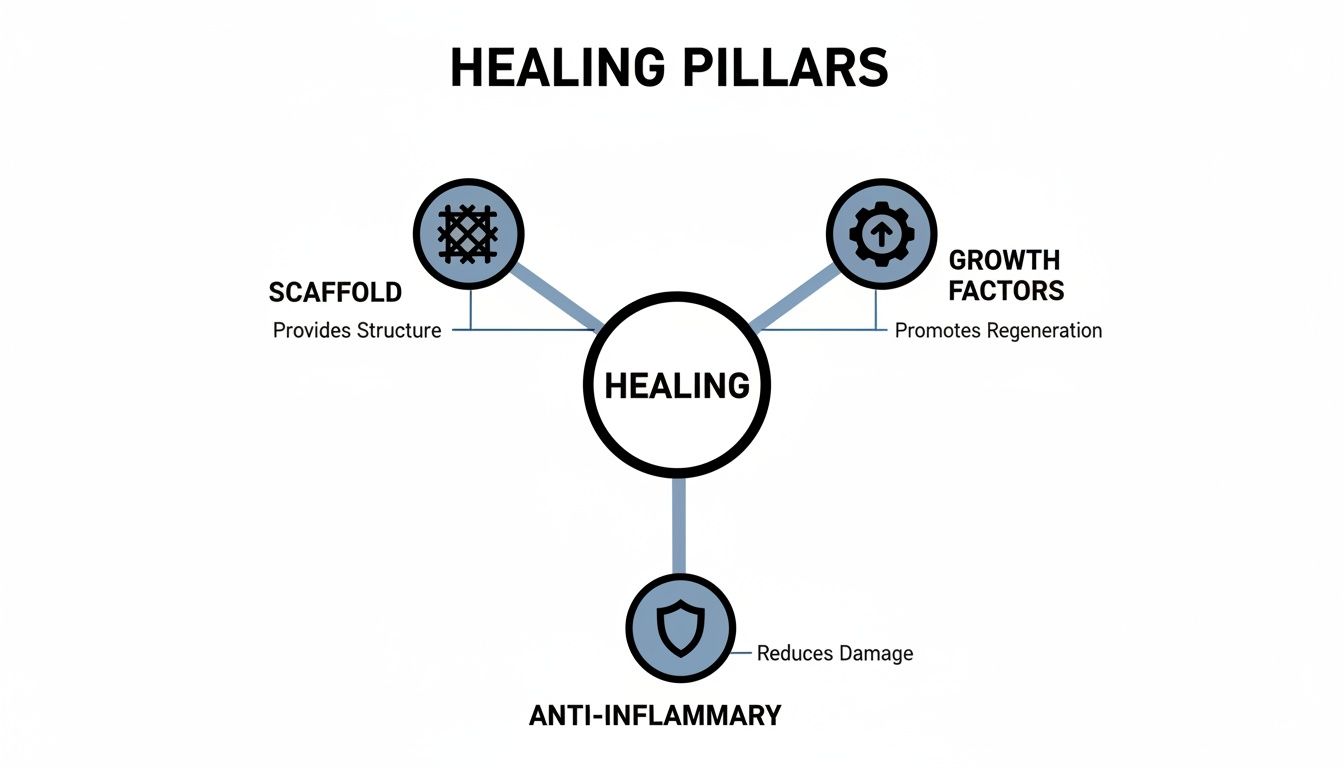
As you can see, the scaffold gives new cells a structure to build on, growth factors provide the instructions for repair, and the anti-inflammatory properties create the right environment for healing to finally begin. Let's look at how this plays out with a few common, challenging wound types.
Addressing Diabetic Foot Ulcers
Diabetic Foot Ulcers (DFUs) are notoriously tough. They're often caught in a perfect storm of poor circulation, nerve damage (neuropathy), and a state of constant, low-grade inflammation. This inflammatory cycle keeps the wound stuck, preventing it from ever moving into the rebuilding phase. This is where amniotic membrane wound healing can be a game-changer.
When we apply an amniotic graft, we're directly fighting that runaway inflammation. The membrane’s potent anti-inflammatory agents help calm the wound bed down, finally breaking the cycle of damage. This gives the growth factors in the graft a chance to get to work, signaling the local cells to start rebuilding healthy tissue.
Patient Story Example: We treated a 68-year-old man with type 2 diabetes who had a non-healing ulcer on the bottom of his foot for over eight months. Despite standard care like offloading and debridement, it just wouldn't close. After just two applications of an amniotic membrane allograft, you could see the inflammation calm down. Healthy granulation tissue started to fill in, and within six weeks, the ulcer was completely gone—preventing a potential amputation.
Managing Venous Leg Ulcers
Venous Leg Ulcers (VLUs) are a different beast altogether. These wounds are caused by failing veins that let blood and fluid pool in the lower legs. This creates a high-pressure, soggy environment that literally drowns the wound in inflammatory fluid, making it almost impossible for cells to do their job.
Here, the amniotic membrane pulls double duty. First, it acts as a biological barrier, helping manage all that excess fluid (exudate) draining from the wound. Second, its anti-inflammatory properties reduce the cellular stress from the constant fluid buildup, which helps restore balance to the wound bed. This gives the body's own repair mechanisms a chance to get a foothold. The scaffold of the membrane also provides a much-needed foundation for new tissue to grow across what are often large, irregularly shaped ulcers.
Improving Post-Surgical Wound Outcomes
After an operation, the goal is always the same: heal quickly with minimal scarring. But some surgical wounds, especially in areas with a lot of tension or in patients with other health problems, can really struggle to close. This can lead to serious complications like an infection or the wound reopening (dehiscence).
Placing an amniotic membrane over a complex surgical incision helps guide a more organized healing process. The graft acts as a protective shield against bacteria while delivering growth factors to promote faster, healthier tissue growth. Its anti-scarring properties are a huge plus, as they help regulate how collagen is laid down. The result is a more flexible, functional, and better-looking scar, which is especially important for joints and other areas where movement is key.
The clinical proof for these applications is solid and continues to grow. Data shows that dehydrated amniotic membrane allografts typically integrate into the wound bed within one to two weeks. By the third week, we often see a noticeable reduction in the wound's size. This rapid integration helps cut down on infection rates and speeds up healing timelines for all kinds of wounds. To get a better sense of the data, you can explore more research on amniotic membrane efficacy and its successful clinical outcomes.
The Patient Journey with Amniotic Membrane Grafts
When you’re dealing with a wound that just won't heal, understanding the "what" and "how" of an advanced therapy is one thing. But knowing what to expect as a patient is just as crucial.
The good news is that receiving an amniotic membrane allograft is often surprisingly simple. It’s designed to be a minimally invasive, in-office procedure that feels more like a collaborative step forward between you and your clinical team than a major medical event.
The entire process begins with a careful evaluation. A wound care specialist will take a close look at your wound—its size, depth, and history—as well as your overall health to see if amniotic membrane wound healing is the right path for you.
Identifying the Right Candidates
So, who is the ideal candidate for this therapy? We’re typically looking for patients with chronic wounds that have hit a wall with standard treatments. These are wounds that are clean and prepped for healing but have simply stalled out.
We often see great success with patients who have:
- Diabetic Foot Ulcers that aren't closing despite proper offloading and regular care.
- Venous Leg Ulcers where compression therapy alone isn't getting the job done.
- Complex Post-Surgical Wounds that are struggling to heal or are at high risk for significant scarring.
Of course, this treatment isn't for everyone. A key contraindication is an active, untreated infection. We also need to ensure there’s adequate blood flow to the area. A clean, well-prepared wound bed is absolutely essential for the graft to work its magic.
What to Expect During Application
Once we've determined you're a good candidate, the application itself is quick and painless. It's done right in the clinic, usually in just a few minutes, with no need for anesthesia or stitches.
Here's how it typically goes:
- Wound Preparation: First, the clinician will gently clean the wound, clearing away any non-viable tissue. This ensures the graft makes direct contact with a healthy surface ready to heal.
- Graft Placement: The dehydrated amniotic membrane is then carefully laid over the entire wound. We position the stromal side—the side packed with healing components—directly against the wound bed.
- Securing the Graft: The graft is secured with simple sterile strips. No stitches required.
- Dressing: Finally, a moist, non-adherent dressing is placed over the graft, followed by a secondary dressing to keep everything clean and protected.
The entire procedure is designed for patient comfort. The amniotic membrane itself acts like a soothing, biological bandage that immediately begins to calm inflammation and reduce pain at the wound site.
The dehydrated amniotic membrane gets to work right away, typically incorporating into the wound bed within 1-2 weeks. It’s not uncommon to see visible signs of improvement in as little as 2-3 weeks. In fact, many US wound centers report up to 50% faster closure for diabetic ulcers using this approach.
Follow-Up Care and Signs of Progress
After the graft is placed, consistent follow-up is key. You'll have regular appointments to monitor your progress and for dressing changes.
During these visits, we’ll be looking for all the right signs: less inflammation, reduced drainage, and the appearance of that healthy, pink granulation tissue that tells us new skin is forming. We can even use advanced imaging to track changes in bacterial load and tissue health. You can learn more in our guide to using a point-of-care wound imaging device.
It's vital to remember that the graft is just one powerful tool in a much larger strategy. To get the best results, we have to pair it with other essential wound care practices—like proper offloading for foot ulcers or consistent compression for venous ulcers. Good nutrition is also critical to fuel the healing from within. This complete, integrated approach is what gives you the very best chance for a full and lasting recovery.
Navigating Reimbursement and Documentation Requirements
Great clinical work is only half the battle when it comes to advanced therapies like amniotic membrane allografts. The other half is mastering the paperwork. Securing reimbursement is absolutely vital to making these treatments accessible for the patients who stand to benefit the most. The entire process comes down to one thing: clear, thorough, and convincing documentation of medical necessity.
Without a strong, evidence-backed story in the patient's chart, even the most clinically sound decision can get shot down by payers. I always tell my team to think of their documentation as building a legal case. Every note, every measurement, and every photo is a piece of evidence proving why this advanced graft wasn't just another option—it was the necessary next step to prevent a far worse outcome.
Proving Medical Necessity
Payers need to see a logical progression that led you to choose an amniotic membrane graft. This means your documentation has to clearly show that you already tried standard, conventional wound care and that it failed to move the needle over a reasonable amount of time, which is typically at least 30 days.
Your notes need to paint a vivid picture of a wound that has stalled out or is getting worse, despite your team providing consistent, appropriate care. This documented history of failed therapies is the foundation of your claim. It shows you took a thoughtful, tiered approach and justifies escalating to a more specialized biologic therapy.
Reimbursement isn't just about plugging in the right billing codes. It's about storytelling. Your documentation has to tell the compelling and accurate story of a chronic wound that simply wouldn't respond to standard care, making the use of an amniotic membrane allograft a clear medical necessity.
The Essential Documentation Checklist
Meticulous and consistent documentation is your single best defense against claim denials. Getting this right is non-negotiable for both patient care and navigating the complex reimbursement landscape. For busy clinicians, tools like healthcare documentation automation can be a huge help in getting this done efficiently.
To build a robust and undeniable case for coverage, make sure every patient chart contains these key elements:
- Detailed Wound Assessment: Document the wound’s specific characteristics at every single visit. This means precise measurements (length, width, and depth), the type and amount of exudate, and a description of the surrounding tissue.
- Photographic Evidence: A picture truly is worth a thousand words to a claims reviewer. Take clear, dated photographs at regular intervals to create a visual timeline of the wound’s failure to progress with standard care.
- History of Failed Therapies: Create a simple, clear timeline of every treatment you used before applying the amniotic membrane. List the specific therapies (e.g., sharp debridement, various dressing types, offloading methods) and how long you tried each one.
- Underlying Comorbidities: Connect the dots between the wound and the patient's overall health. Document conditions like diabetes, peripheral artery disease, or venous insufficiency that are making the wound so difficult to heal.
- Specific Billing Codes: This is a big one. You have to use the correct Healthcare Common Procedure Coding System (HCPCS) "Q-codes" that match the exact amniotic membrane product you used. Accuracy here is critical to avoid simple, frustrating administrative denials.
By diligently including these components in every chart, you create an unassailable record that backs up your clinical judgment and dramatically increases the likelihood of getting the claim paid.
Integrating Amniotic Membranes into Advanced Wound Care
Amniotic membrane allografts are a powerful tool in our arsenal, but it's a mistake to think of them as a standalone "magic bullet" for every non-healing wound. Their real power is unlocked when they're intelligently woven into a modern, comprehensive wound care strategy.
Think of it like a master craftsman bringing in a specialized tool at the perfect moment to overcome a stubborn obstacle in a larger project. The art and science of advanced wound care are all about knowing precisely when to deploy these grafts. They're most effective not at the very beginning of treatment, but at a critical inflection point—after the wound has been properly cleaned and prepped, but has hit a frustrating plateau.
This strategic timing is everything. Applying a graft to a wound that's still full of unhealthy tissue or has an uncontrolled bacterial load is like trying to plant a prize-winning rose in a bed of weeds. It just won’t take.
The Right Tool at the Right Time
A skilled wound care team always starts by establishing a clean, healthy foundation in the wound bed. This foundational work involves meticulous debridement, getting any infection under control, and making sure there's adequate blood flow to the area.
Only when that foundation is solid, but the wound has visibly stalled, does the amniotic membrane enter the picture. At this specific stage, the graft acts as a potent catalyst. It provides the biological jumpstart needed to nudge the wound out of its chronic, inflammatory state and back into an active healing phase. The prepared wound bed is now perfectly primed to receive the growth factors and scaffold the graft delivers.
This patient-focused, evidence-based approach ensures that advanced tools are used to solve specific problems, moving us far beyond a one-size-fits-all mentality. It's all about pinpointing and addressing the unique barriers preventing each individual wound from closing. This is a core principle behind the advanced treatment options at Specialty Wound Care, where every therapy is one piece of a larger, coordinated plan.
An amniotic membrane graft is rarely the first step in wound care, but it's often the critical one that bridges the gap between a clean wound and a fully closed one. Its success is a direct result of a well-executed, holistic treatment strategy.
Achieving Durable Closure and Better Quality of Life
By integrating amniotic membranes into a broader care pathway, we can achieve outcomes that are both faster and more durable. The goal isn't just to close the wound, but to rebuild strong, functional tissue that's far less likely to break down again in the future.
This integrated model involves several key components working in synergy:
- Initial Wound Bed Preparation: Thorough cleaning, debridement, and infection management create the ideal environment.
- Strategic Graft Application: Applying the amniotic membrane only once the wound is clean but has stopped progressing.
- Supportive Therapies: Continuing essential care, like offloading for foot ulcers or compression for venous leg ulcers.
- Nutritional Support: Making sure the patient has the protein and nutrients required to fuel tissue regeneration.
When all these elements come together, the result is so much more than just a healed wound. It’s a restored quality of life for patients who were previously stuck in a demoralizing cycle of pain and frustration. This intelligent, multi-faceted approach is the future of effective wound management.
Common Questions About Amniotic Membrane Healing
When you're dealing with a wound that just won't heal, exploring advanced options like amniotic membrane allografts is a smart move. But it's natural to have questions. Here are some straightforward answers to what patients most often ask us.
Is the Application Painful?
This is usually the first thing people want to know, and the answer is reassuring. Applying an amniotic membrane graft is a gentle, in-office procedure. We simply clean the wound, lay the thin, flexible graft over the surface, and secure it. Most patients tell us they feel little to nothing during the process.
In fact, the opposite is often true—many people feel less pain after the graft is in place. The membrane is packed with powerful anti-inflammatory agents that get to work right away, calming the wound site and often providing a welcome sense of relief.
How Safe Are Amniotic Membrane Grafts?
Patient safety is always our number one priority. The amniotic tissue comes from healthy, consenting mothers who donate it after a scheduled Cesarean section. Every donor goes through a comprehensive screening process, similar to what's required for blood donation, to ensure they are free of any communicable diseases.
From there, the tissue is processed in a sterile lab following strict standards set by the American Association of Tissue Banks (AATB) and the FDA. This meticulous process guarantees that every allograft is sterile and safe for clinical use, minimizing any risk of infection or rejection.
How Many Treatments Will I Need?
This really depends on your specific wound—its size, its history, and how it responds to the first treatment. For a lot of chronic wounds, a single application is all it takes to provide that biological "jumpstart" needed to get the healing process back on track and moving toward full closure.
However, for bigger or more stubborn wounds that have been around for a long time, a second or third application might be recommended. Your specialist will keep a close eye on your progress. If healing starts to plateau after a few weeks, another graft can help maintain that forward momentum. The goal is always the same: to get you healed completely and durably with the fewest steps possible.
At Specialty Wound Care, we don't just apply a product; we integrate these advanced allografts into a complete, evidence-based treatment plan. Learn how our patient-centric approach accelerates healing and restores quality of life.
