Wound care is more complex than ever, yet many treatments still miss key details that slow healing. You know expert wound assessment matters, but pairing it with technology like MolecuLight DX brings a new level of precision. This combination sharpens diagnosis, targets therapy, and sets a clear path to better wound healing outcomes. Read more.
Enhancing Diagnostic Accuracy

The union of expert evaluation and advanced tools refines diagnostics, ensuring precise identification and treatment.
Expert Wound Assessment Techniques
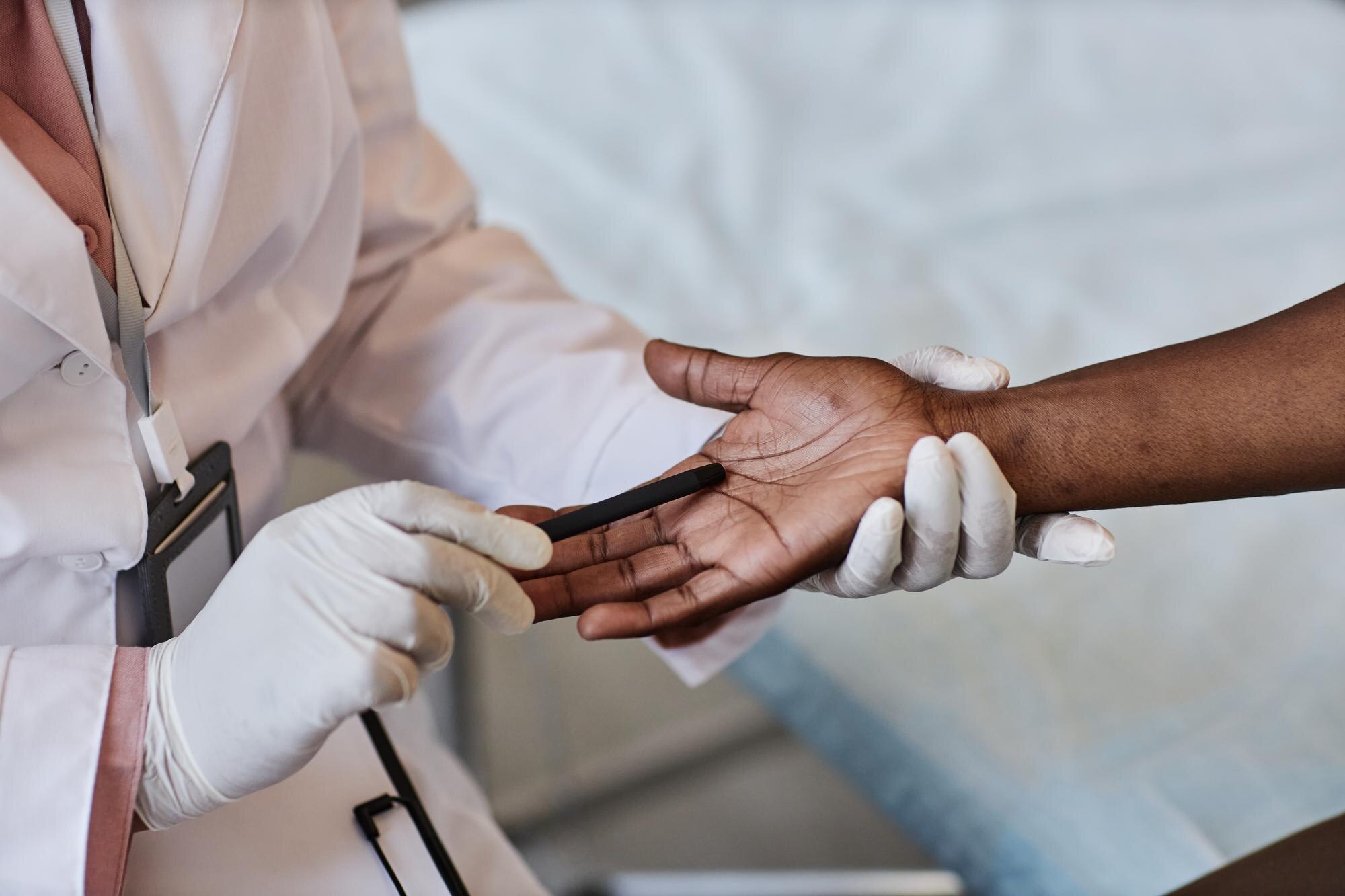
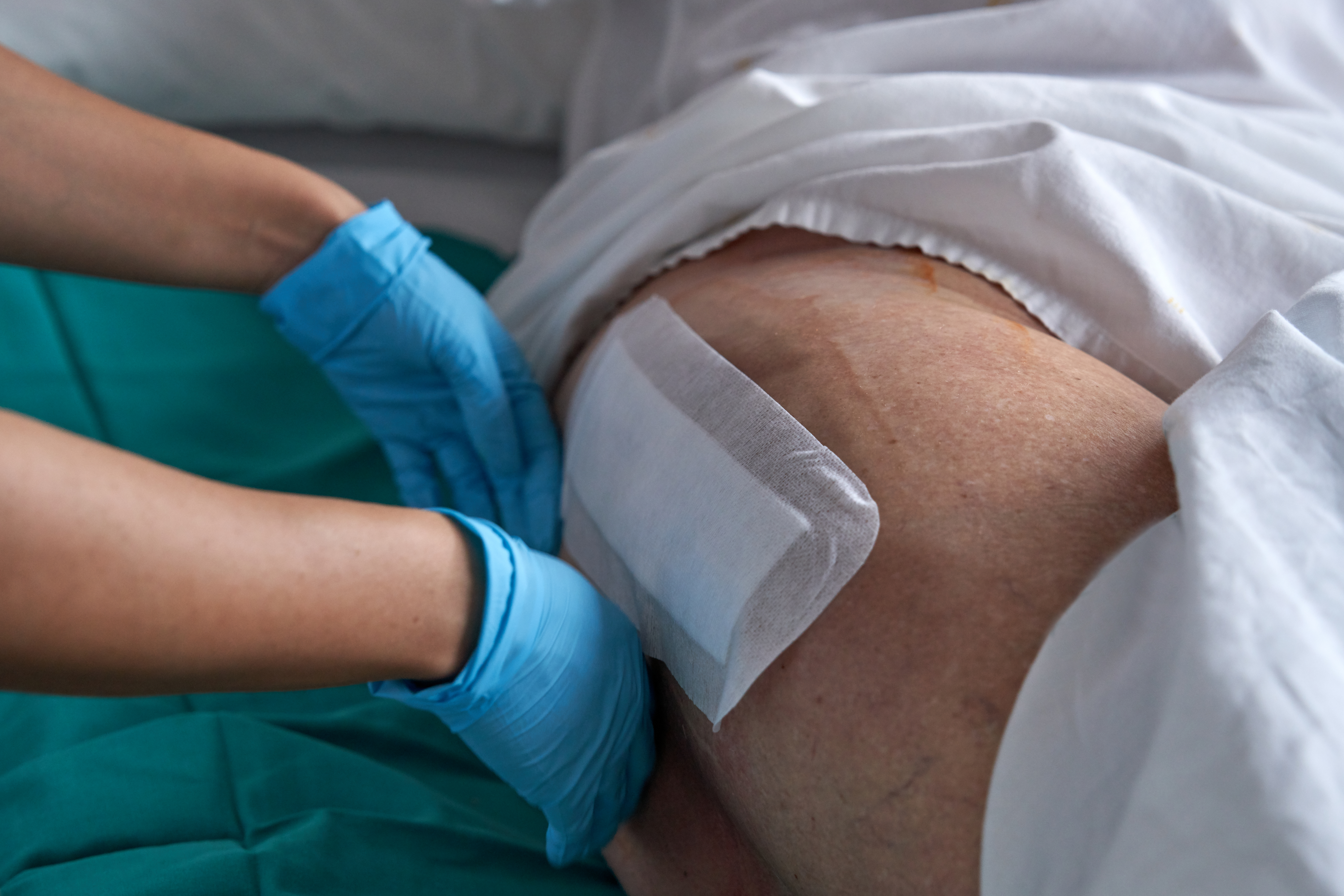
Your expertise in wound assessment is crucial. It’s all about observing the wound, noticing changes, and understanding its needs. Look closely at the wound bed: is it red, yellow, or black? Each color tells a story. A red wound might be healing, while a black one might need cleaning. Check for edges, too. Rolled edges can slow down healing. Focus on these little things. They’re not just details; they’re keys to choosing the right path for healing. Remember: every wound has a tale to tell.
Advanced Wound Care Technologies
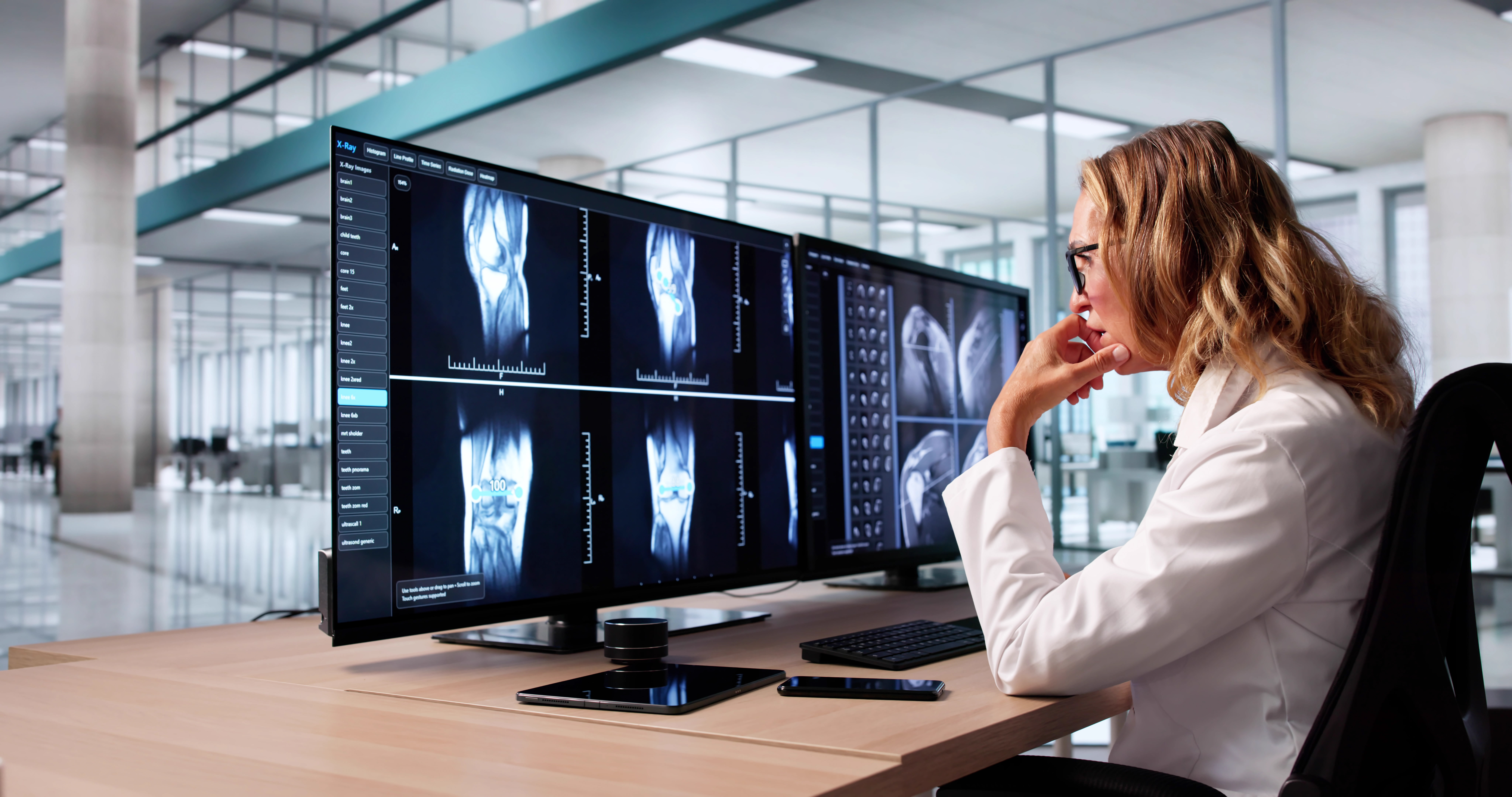
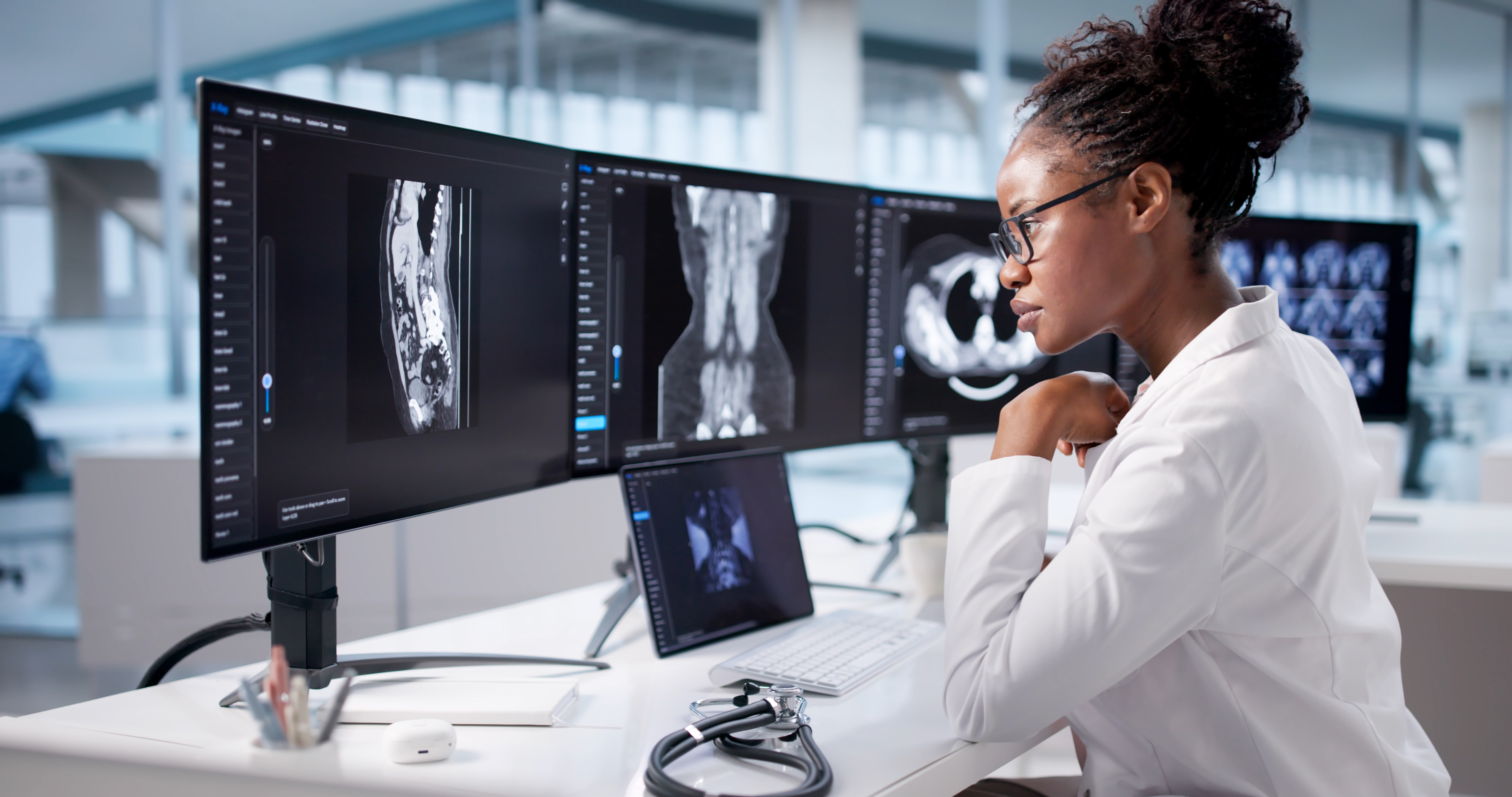
Having cutting-edge tools at your fingertips makes a difference. Imagine using something that gives you a clear view of what’s hidden beneath. Devices that measure size, shape, and depth can help you track real changes over time. It’s like having a magnifying glass for wounds. These tools don’t just save time. They give you solid, reliable data. When you’re equipped with the best technology, you’re not just treating wounds. You’re leading the way in care. That’s what makes a difference.
MolecuLight DX and Bacterial Fluorescence Imaging
Bacterial fluorescence imaging shines a light on the unseen. With MolecuLight DX, you peek into the bacterial world of a wound. This device shows you bacteria in real-time. No waiting for lab results. You know instantly where bacteria thrive. It even helps guide cleaning and treatment. By doing so, it cuts down on trial and error in therapy. Using this tool, you’re not just reacting. You’re acting with precision. That’s not just smart care; it’s next-level care.
Guiding Targeted Therapy

With accurate diagnostics, therapy becomes more focused and effective, addressing specific challenges faced by wounds.
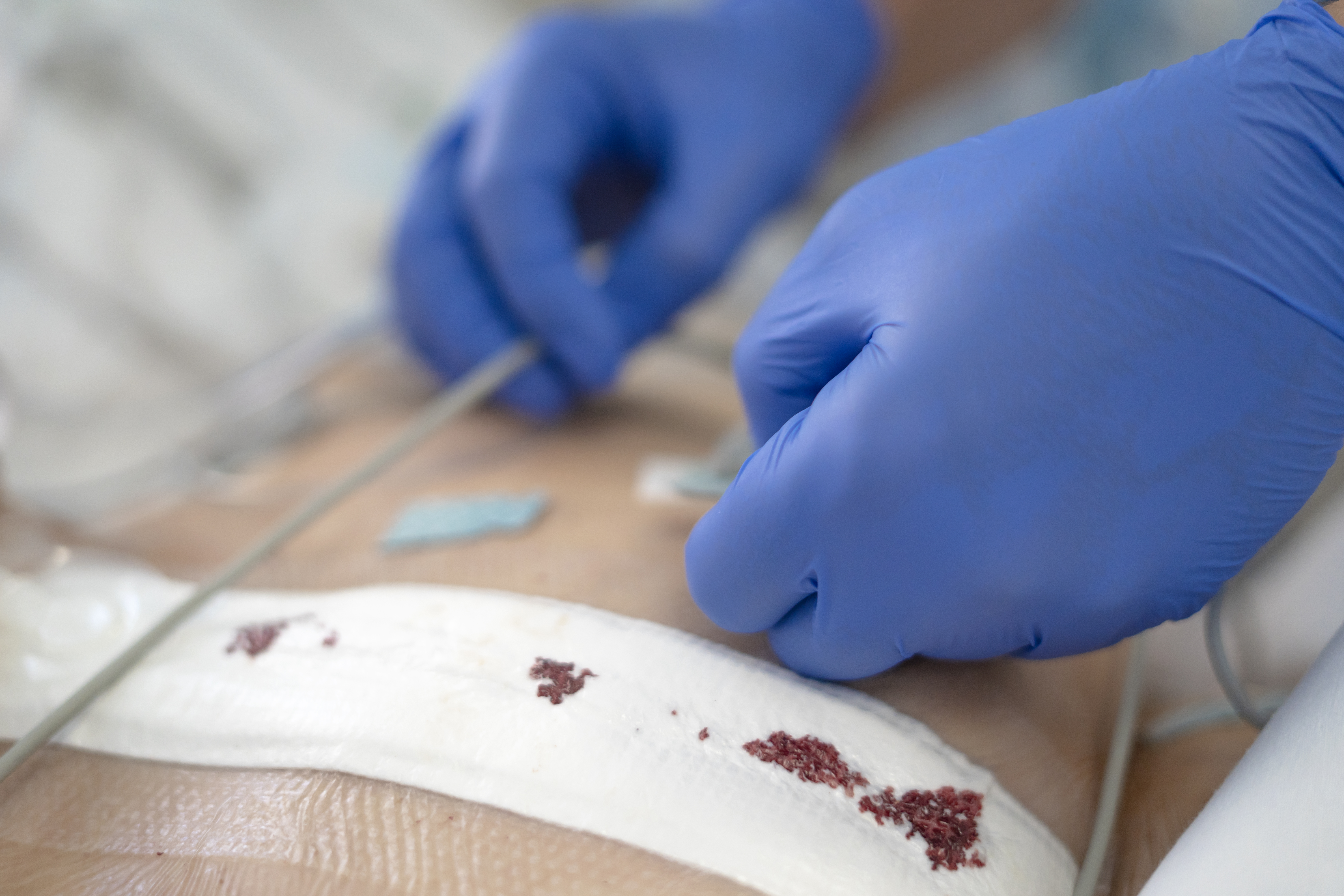
Biofilm Detection and Pathogen Testing
Biofilms are tricky barriers. They protect bacteria, making them tough to treat. Detecting them early is crucial. Use specialized tests that spotlight these hidden foes. They tell you which pathogens are present. Equipped with this knowledge, you choose the right medicine quickly. No guesswork. This precision can prevent delays in healing. Biofilm detection is not just about finding bacteria. It’s about clearing the path to healing.
Triple-Layer Allograft for Grafting
Your wound healing toolkit just got an upgrade. The triple-layer allograft is a standout option. It’s crafted from three layers, giving it strength and flexibility. When grafted, it acts as a scaffold, supporting native tissue. This allograft is made following strict guidelines, ensuring safety and effectiveness. It merges seamlessly with the body’s natural healing process. Choosing this option means opting for a reliable, trusted solution. Transform your grafting with this advanced choice.
Personalized Treatment Plans
Every wound is unique. That’s why a one-size-fits-all approach doesn’t work. Crafting a personalized plan is key. Start by gathering all details: wound type, patient’s health, and potential complications. With this information, tailor a plan that meets the wound’s specific needs. Regular check-ins allow for adjustments based on progress. This dynamic approach ensures each step is aligned with healing goals. Personalized plans are not only effective but empower you with a roadmap to success.
Improving Healing Outcomes

When therapies are guided well, the journey towards recovery becomes smoother, leading to improved patient outcomes.
Diabetic Foot Ulcer Care Strategies
Diabetic foot ulcers require close attention. High blood sugar can slow healing. Start with controlling blood sugar levels. Next, focus on pressure relief. Special shoes or inserts can help. Regular check-ups are essential. Look for signs of infection or worsening. Early intervention can prevent complications. Preventive care, combined with these strategies, supports better healing outcomes. You’re not just managing wounds. You’re enhancing lives.
Venous Leg Ulcer and Pressure Injury Management
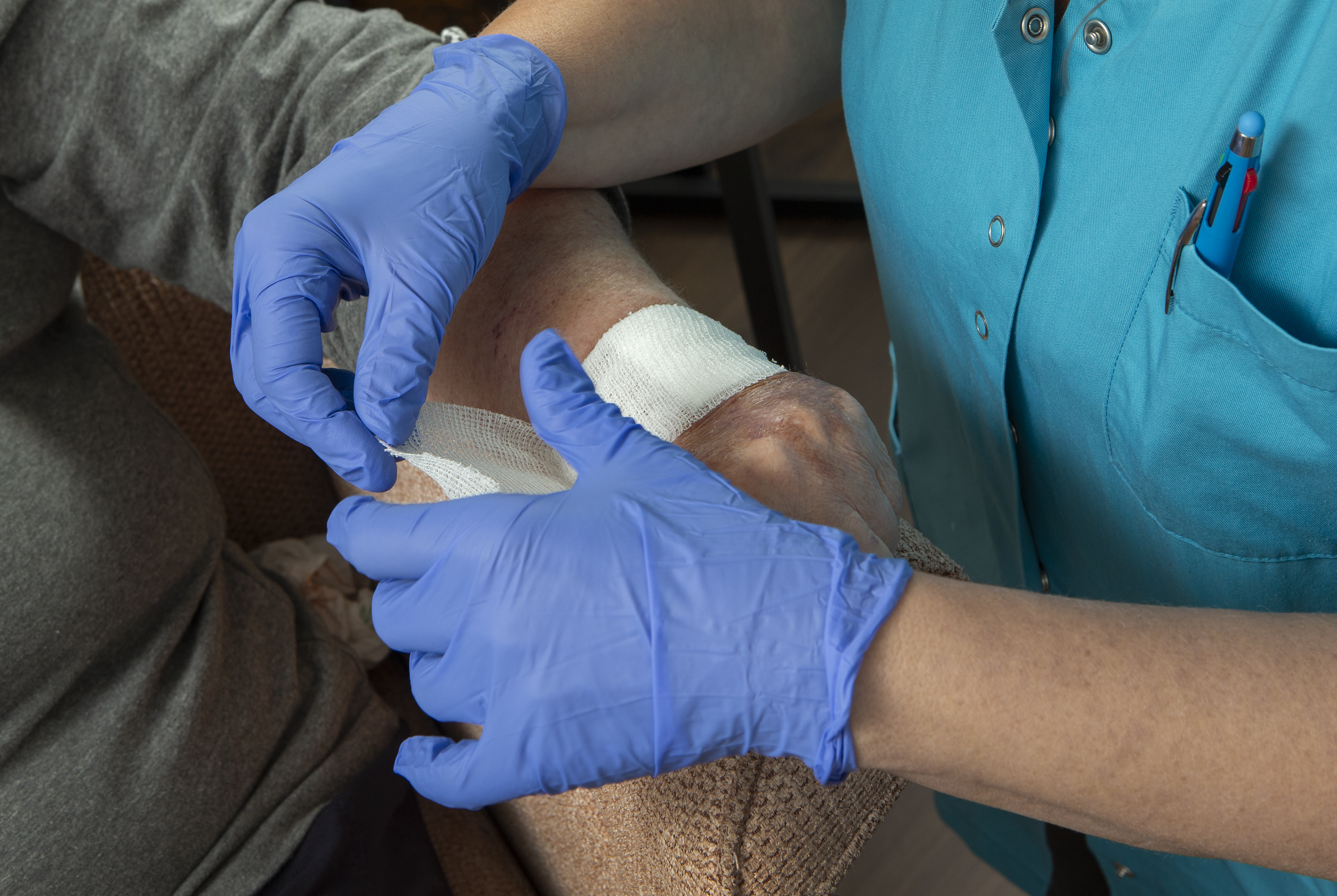
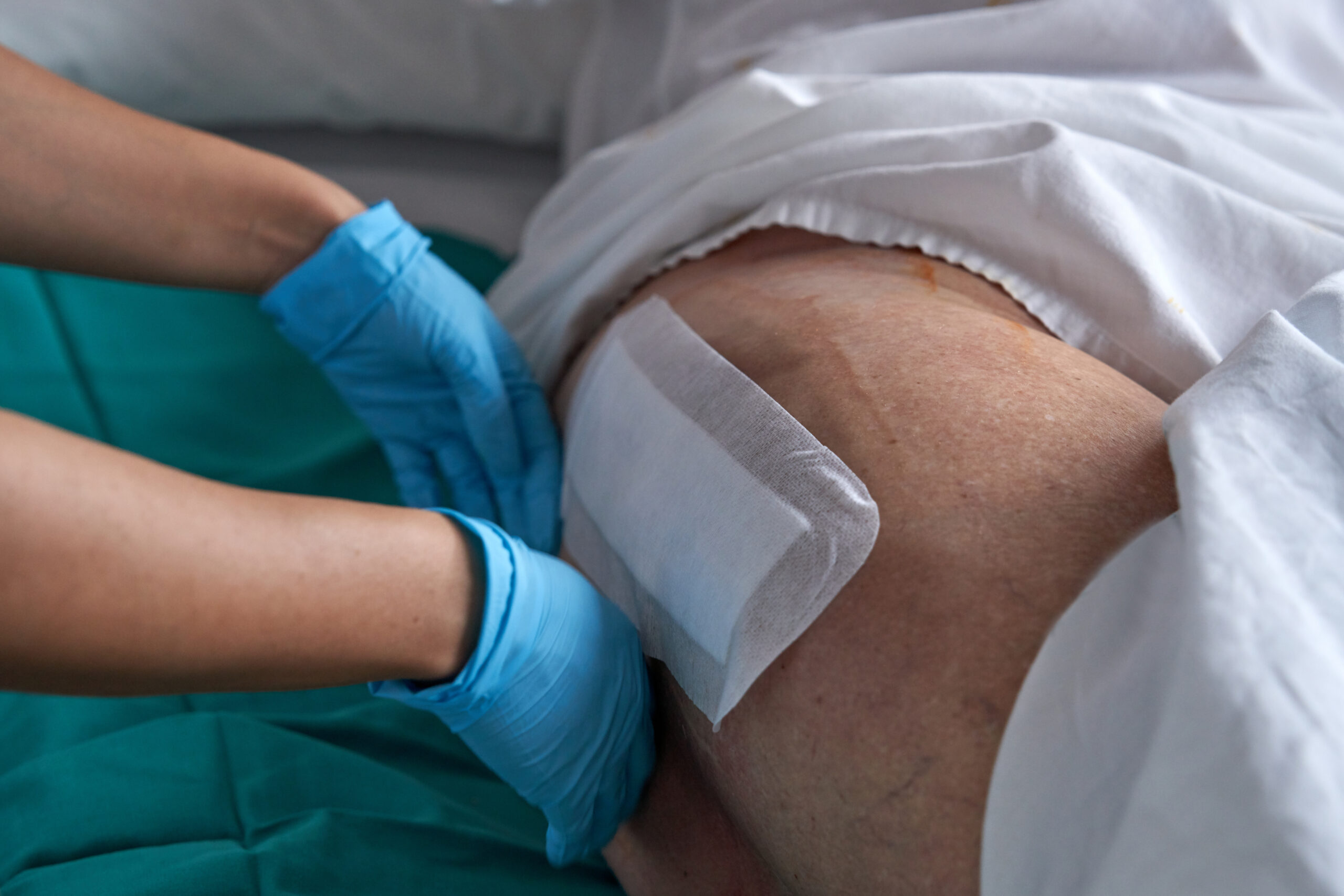
Managing these ulcers requires a two-pronged approach. First, address the root cause: poor circulation. Compression therapy can boost blood flow. Second, focus on wound care. Clean and dress wounds regularly. Use advanced products that support healing, like special bandages that keep the area moist. Regular assessments help track progress. By combining these strategies, you can turn a challenging situation into a manageable one. It’s about creating an environment where healing thrives.
Comprehensive Wound Documentation Technology
Documentation is more than just note-taking. It’s a vital tool in wound care. Use technology that captures every detail. Photos, measurements, and changes can be logged efficiently. This not only helps in tracking progress but also ensures everyone involved is on the same page. When team members see the same data, care becomes more consistent. Comprehensive documentation supports informed decisions, paving the way for better outcomes. It’s the backbone of effective wound management.
Discover how our solutions outperform standard treatments—contact us for a demo.