Innovations in Wound Care: Imaging, Allografts, and Precision Testing
Conventional wound care often falls short when treating chronic wounds like diabetic foot ulcers and pressure injuries. You know how frustrating it is when healing stalls despite your best efforts. Innovations in wound care now offer tools like MolecuLight DX fluorescence imaging and triple-layer allografts to catch infection early and support tissue repair. Let’s explore how these advances can improve outcomes for your patients and streamline your practice. For more information, you can check this link.
Cutting-Edge Imaging Techniques
State-of-the-art imaging can greatly enhance wound care by providing outstanding insight into wound conditions. These advances allow for quicker and more accurate assessments.
Role of Fluorescence Imaging
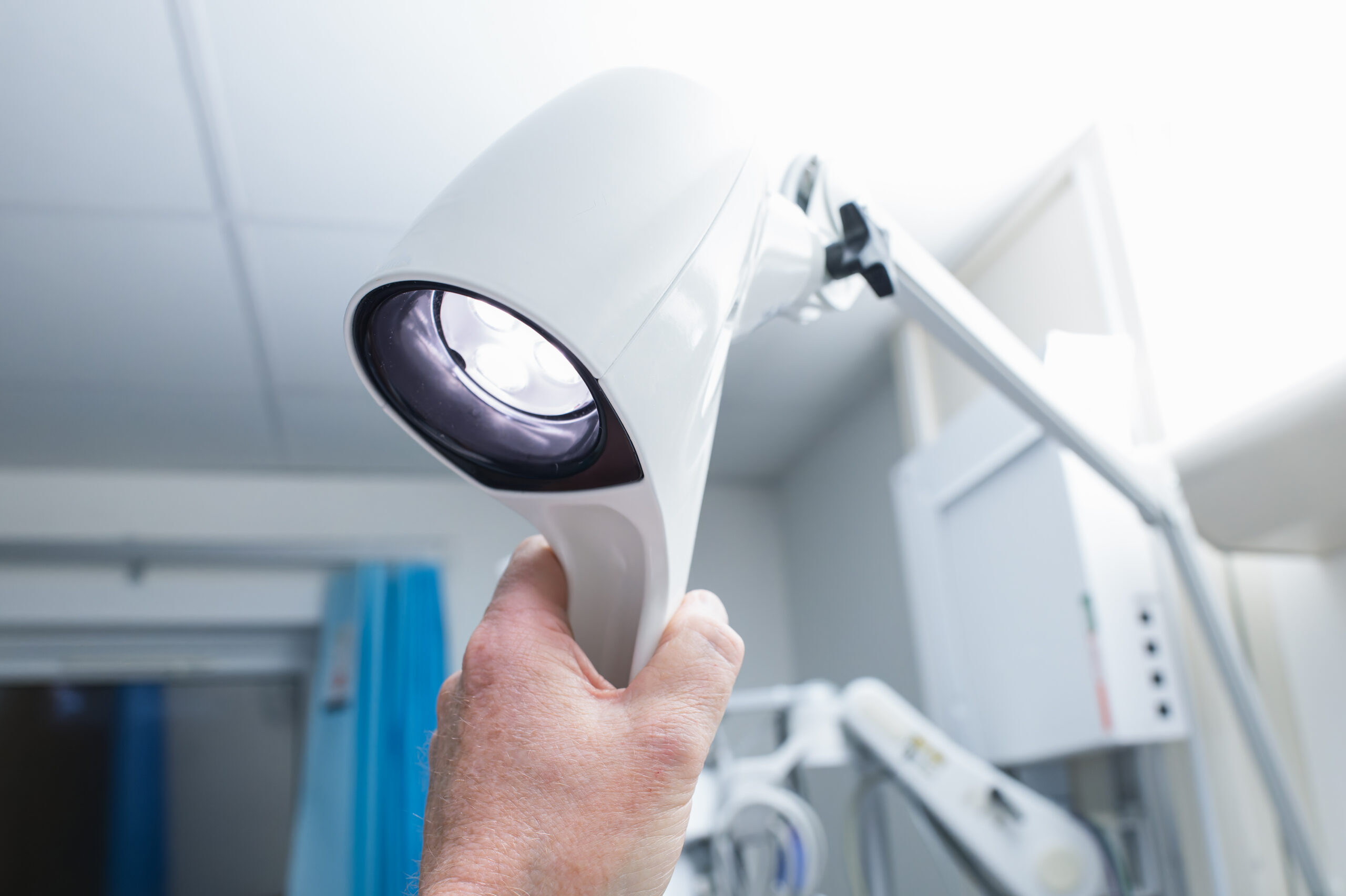
Fluorescence imaging reveals hidden details of wounds that you might otherwise miss. This technique highlights areas of concern by illuminating bacterial presence. When you use it, you can identify problems earlier, which can be crucial for treatment success.
This method stands out because it shows you the bacterial burden without needing direct contact with the wound. By shining a specific light, fluorescence imaging provides a visual map of bacteria in real-time. This means faster decisions and more targeted care. You gain a clear advantage in treating complex cases, like diabetic foot ulcers and venous leg ulcers.
Detecting Bacterial Burden with MolecuLight DX
MolecuLight DX is a powerful tool in your wound care arsenal. It helps you spot bacteria that might not be visible otherwise. This device uses light to reveal the bacterial load, giving you a clearer picture of what you’re dealing with.
Using this tool, you gain immediate feedback. It reduces the guesswork in identifying infection hotspots. With this knowledge, you can tailor your treatments more effectively. Imagine detecting an infection before it spirals out of control: that’s what MolecuLight DX offers. This not only improves patient outcomes but also enhances your practice’s efficiency.
Advanced Skin Substitute Solutions

When traditional dressings aren’t enough, advanced skin substitutes come into play. These modern solutions offer significant benefits in wound management.
Benefits of Triple-Layer Allograft
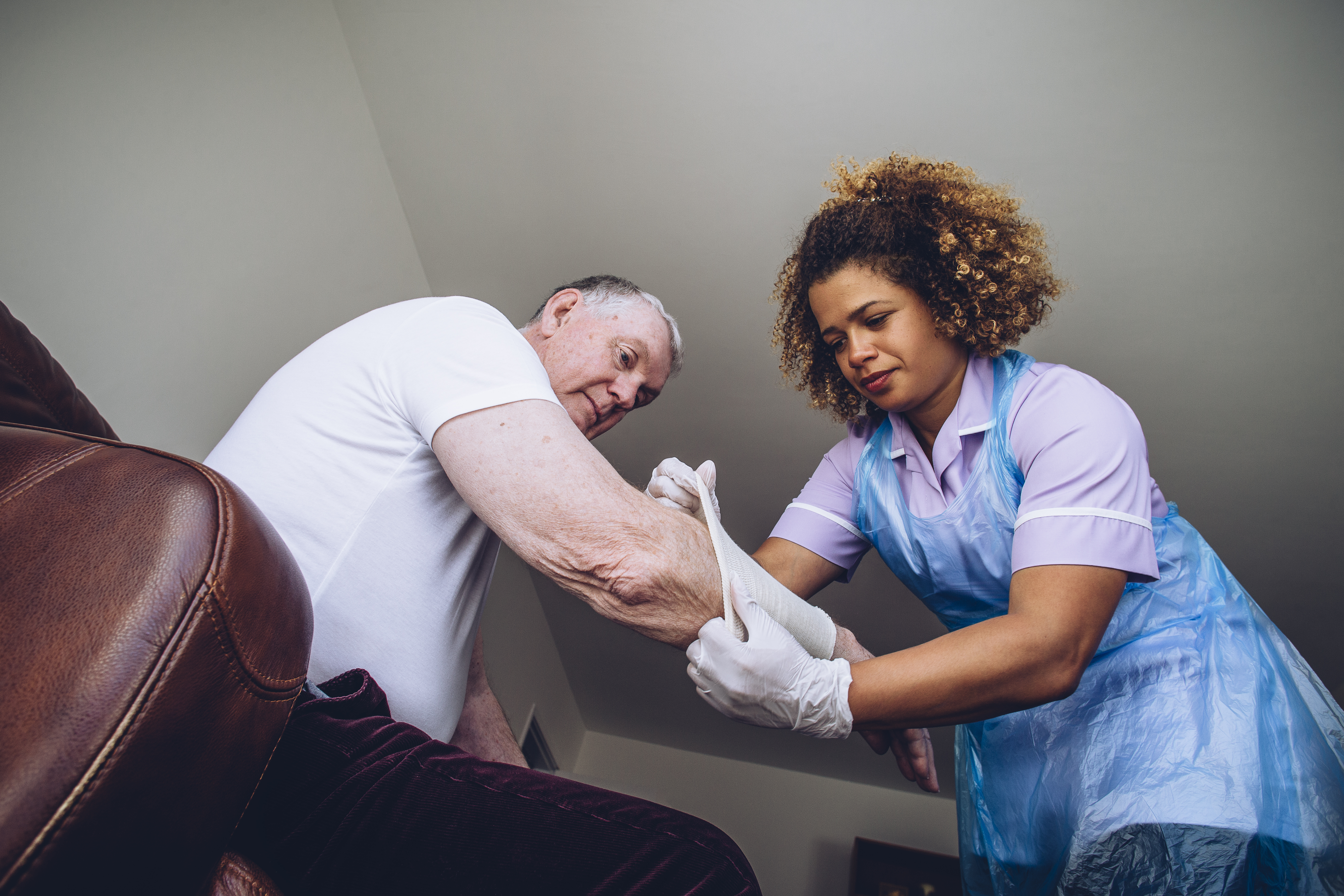
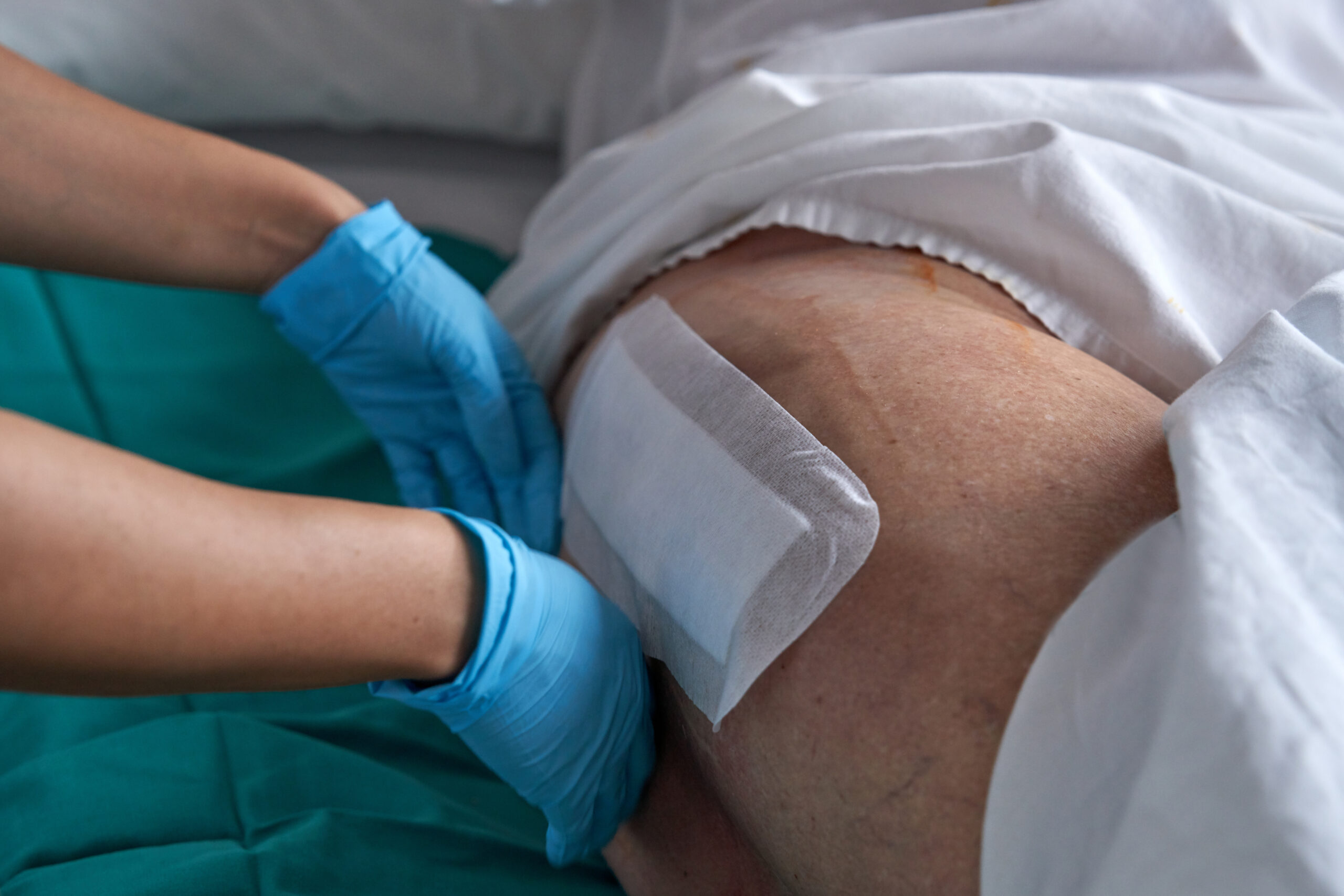
Triple-layer allografts are game-changers in wound healing. They provide a scaffold that supports tissue regeneration. This structure mimics natural skin layers, promoting faster healing.
The allograft is made from carefully selected and screened materials, ensuring safety and effectiveness. It assists in closing wounds more rapidly, reducing the risk of complications. For pressure injuries and chronic wounds, this can mean the difference between prolonged treatment and swift recovery.
Cellular and Tissue-Based Products (CTPs)
CTPs are designed to enhance healing where conventional methods fall short. These products incorporate living cells that assist in tissue repair and regeneration.
CTPs offer a dynamic treatment option. They can be tailored to fit the needs of complex wounds like venous leg ulcers. With their ability to integrate seamlessly with your patient’s natural tissues, they provide a reliable option for difficult-to-heal wounds. The science behind CTPs means they not only close wounds but do so with a stronger, healthier skin structure.
Precision Testing and Therapy
Pinpoint testing and therapy bring a new level of precision to wound care, allowing you to treat wounds more effectively and efficiently.
Targeted Antimicrobial Therapy
When you know exactly what pathogens are present, you can choose the right treatment. Targeted antimicrobial therapy focuses on using specific medications that tackle identified bacteria.
This precise approach minimizes the use of broad-spectrum antibiotics, which can lead to resistance. By targeting the exact bacteria, you not only improve healing rates but also protect your patients from unnecessary drug exposure. This method is particularly useful in tackling complex infections that don’t respond to standard treatments.
Importance of Rapid Advanced Testing Methods
Quick and accurate testing is crucial in wound management. Advanced methods provide you with results far faster than traditional techniques.
These tests can identify pathogens in hours rather than days. This speed allows for rapid initiation of appropriate treatments. The result is a more effective management strategy that benefits both you and your patients. With fast testing, you can adapt your approach swiftly, improving recovery times and reducing hospital stays.
In summary, utilizing these innovations in wound care can significantly enhance your practice. By integrating imaging, advanced skin substitutes, and precision testing into your routine, you can offer superior care to your patients. For more insights, check out this blog.
Discover how our solutions outperform standard treatments—contact us for a demo.