When it comes to preventing diabetic foot ulcers, nothing beats a consistent, proactive daily foot care routine. This isn't optional; it's a non-negotiable habit. For many of my patients, this simple, five-minute practice is the line in the sand between lasting foot health and a serious, life-altering complication.
The daily trifecta is inspection, cleansing, and moisturizing.
Building Your Daily Foot Protection Routine

The real foundation of ulcer prevention isn't found in a high-tech medical procedure. It's built in the quiet, consistent habits you form at home. With diabetes, especially if neuropathy has dulled your ability to feel pain, a tiny problem can escalate into a major threat almost overnight. A dedicated daily routine makes you the first line of defense.
Think of it as your personal "3-minute drill" for limb preservation. It’s a moment to check in with your body and catch trouble before it ever gets a foothold. For those who might struggle with self-care due to mobility issues or other health challenges, understanding what a home health aide is can open up new avenues for maintaining this crucial daily routine and overall wellness.
The Art of the Daily Inspection
Your eyes are your most powerful tool. Since diabetic neuropathy can completely mask injuries, a thorough visual check is the only way to catch issues you literally cannot feel. This isn't just a quick glance; it requires a systematic approach.
- Good Lighting is a Must: Sit in a well-lit room where you can see every part of your feet without shadows.
- A Mirror is Your Best Friend: An unbreakable, long-handled mirror is perfect for examining the bottoms of your feet and heels—areas that are otherwise impossible to see on your own.
- Check Everywhere: Look for anything out of the ordinary—blisters, cuts, scratches, redness, or swelling. Pay special attention to the areas between your toes, a common spot for moisture to build up and cause skin breakdown.
- Feel for Temperature Changes: Use the back of your hand to check for any spots that feel unusually hot or cold. A "hot spot" can be a sign of inflammation or a budding infection long before you see anything.
This daily check is your personal early warning system. Finding a small red spot or a blister today means you can address it immediately, stopping it from ever becoming a dangerous ulcer.
Proper Washing and Drying Techniques
Good hygiene isn't just about being clean; it's about creating an environment where your skin can thrive and fight off infection. Washing your feet the right way is a huge part of ulcer prevention.
Always use lukewarm water—never hot—and a mild soap. If you have neuropathy, you might not realize the water is hot enough to cause a burn. After washing, the drying process is arguably the most critical step.
The spaces between the toes are especially vulnerable to fungal infections and skin breakdown if they stay damp. Gently pat your feet dry with a soft towel, taking extra care to dry thoroughly between each and every toe.
Moisturizing for Skin Integrity
Dry, cracked skin is like leaving the door wide open for bacteria. Moisturizing every day helps maintain a strong, flexible skin barrier that is far less likely to break.
Apply a thin layer of a podiatrist-approved lotion or cream to the tops and bottoms of your feet. But there's one crucial exception: never put lotion between your toes. The extra moisture trapped in that area can encourage fungal growth, creating the exact problem you're trying to prevent.
Nail Care That Prevents Problems
I've seen it countless times: improper nail trimming is a frequent cause of ingrown toenails, which can get infected and quickly lead to an ulcer. The right technique is simple but absolutely vital.
- Cut your toenails straight across.
- Don't cut them too short or try to round the corners.
- Use an emery board to gently file any sharp edges.
If you have thick nails, poor eyesight, or just have trouble reaching your feet, it is much, much safer to have a podiatrist trim your nails. This simple appointment removes a major risk factor and is a smart investment in your health.
Why Your Choice in Footwear Is a Medical Decision

For anyone living with diabetes, thinking of shoes as just another fashion accessory is a dangerous mistake. Your footwear is a medical device—a critical tool in your arsenal for preventing diabetic foot ulcers.
A shoe that rubs, pinches, or creates even a little bit of pressure can quickly lead to a blister or sore. With neuropathy in the mix, you might not even feel it until it has already become a serious wound.
This isn’t hyperbole. The wrong shoe can completely undermine all the hard work you put into your daily foot care routine. It creates constant, low-grade trauma on vulnerable skin, paving the way for breakdown and infection. On the flip side, the right shoe acts as a protective shield, distributing pressure evenly and guarding your feet against the hazards of daily life.
The Anatomy of a Protective Shoe
When you're choosing footwear, you have to look past the style and zero in on specific protective features. Therapeutic shoes designed for diabetic feet are engineered from the ground up to minimize risk. They aren't just about comfort; they are built for safety.
Look for these key characteristics:
- A Wide Toe Box: This is absolutely non-negotiable. A wide, deep space for your toes keeps them from getting cramped, which cuts down on friction and prevents problems like hammertoes from getting worse.
- Seamless Interior: Any seam on the inside can act like sandpaper against sensitive skin, creating a friction point that can easily become a sore. A smooth, seamless lining is essential.
- Extra Depth: This feature lets your foot sit comfortably without pressure on top. It also provides that crucial extra space for custom orthotics or inserts if you need them.
- Supportive, Cushioned Soles: A firm sole protects the bottom of your foot from sharp objects, while good cushioning helps absorb shock and distribute pressure away from high-risk spots like the ball of your foot.
Think of it this way: a regular shoe is like a standard car, but a therapeutic shoe is an armored vehicle designed specifically to protect its precious cargo—your feet.
Getting the Right Fit Every Time
An expensive therapeutic shoe is completely useless if it doesn't fit properly. Getting a professional fitting is one of the most important investments you can make in your foot health. Foot size and shape can change over time, especially with conditions like diabetes.
Here’s a practical tip I give all my patients: Always shop for shoes in the late afternoon or evening. Your feet naturally swell throughout the day. Fitting them when they are at their largest ensures you won't buy a pair that becomes painfully tight by the end of the day.
When you try on shoes, make sure you're wearing the same type of socks you normally would. You should have about half an inch of space—roughly a thumb's width—between your longest toe and the end of the shoe. And never assume your size is the same across different brands. A size 10 in one brand might fit like a 9.5 in another.
Offloading Pressure with Custom Insoles
One of the most critical concepts in preventing foot ulcers is offloading. In simple terms, this just means reducing or redistributing pressure from those vulnerable, high-pressure areas of your foot. Even in the best shoes, certain spots naturally bear more weight than others.
This is where custom orthotics and insoles come into play. A podiatrist can create inserts molded specifically to the unique contours of your feet. These devices provide targeted cushioning and support, effectively offloading the pressure points that are most prone to ulceration.
The science here is solid. Therapeutic footwear and custom insoles aren't just for comfort; they are evidence-based medical interventions that dramatically lower the risk of an ulcer returning.
For instance, studies consistently show that using therapeutic footwear and offloading devices can reduce ulcer recurrence by a remarkable 20% to 40% compared to wearing standard shoes. The data is clear: when patients switch to footwear that cuts peak plantar pressure by at least 30%, their risk of an ulcer returning within a year drops significantly. You can explore the detailed research behind these offloading strategies to understand their powerful impact.
Ultimately, choosing your footwear is an active part of your diabetes management plan. It’s a daily decision that directly impacts your risk of developing a foot ulcer. By investing in professionally fitted, therapeutic shoes and understanding the power of offloading, you transform a simple purchase into a powerful act of prevention.
Connecting Total Diabetes Management to Foot Health
It’s easy to think that diabetic foot care is just about, well, your feet. But that’s a dangerous oversimplification. I’ve seen time and again that the most powerful strategies for preventing foot ulcers start far away from the foot itself—they begin with how you manage your diabetes every single day.
The truth is, your body is one big interconnected system. Consistently high blood sugar, or hyperglycemia, isn't just a number on a meter; it creates a toxic internal environment. It slowly poisons your nerves and blood vessels, setting the perfect stage for the two main culprits behind ulcers: diabetic neuropathy and peripheral artery disease.
How High Blood Sugar Sets the Stage for Ulcers
Think of it this way: when blood glucose stays high, it attacks the delicate nerve endings, especially in your hands and feet. This is diabetic neuropathy. It can completely wipe out your ability to feel pain, heat, or cold. Your foot becomes a numb landscape where injuries simply go unnoticed. A small rock in your shoe, a blister from a new pair of loafers—these can exist for days without you feeling a thing.
At the same time, all that excess sugar is damaging the lining of your arteries, causing them to harden and narrow. This is peripheral artery disease (PAD), and it dramatically chokes off the flow of oxygen-rich blood to your feet. Poor circulation means that any small wound, like that blister you never felt, can't get the resources it needs to heal.
This combination is the perfect storm for an ulcer. Neuropathy lets an injury happen without you knowing, and PAD stops your body from healing it. This changes the game completely. Foot care isn't just about what you do to your feet, but what you do for your entire body.
Glycemic Control: Your Primary Defense
This brings us to the single most important thing you can do to protect your nerves and vessels: keep your blood glucose levels stable. This isn't about chasing a single "perfect" reading. It's about staying within your target range as consistently as possible. In fact, effective total diabetes management is the cornerstone of foot ulcer prevention. For some practical, actionable advice, you can explore these 8 Proven Ways to Stabilize Blood Sugar Levels.
Getting there requires a multi-pronged attack:
- Mindful Nutrition: Focus on a diet packed with fiber, lean proteins, and healthy fats. Being smart about your carbohydrate intake helps prevent those sharp blood sugar spikes that do so much damage over time.
- Consistent Physical Activity: Regular exercise, even just a daily walk, makes your body more sensitive to insulin and helps lower your blood glucose.
- Medication Adherence: Whether you're on pills, insulin, or other injectables, take them exactly as prescribed. They're a critical tool for keeping your glucose levels where they need to be.
Think of stable blood sugar as a protective shield for your entire circulatory and nervous system. Your feet are just one of the biggest beneficiaries.
Every single time you make a healthy food choice, take your medication on schedule, or go for that walk, you are actively preventing a foot ulcer. It’s a direct cause-and-effect relationship.
The Overlooked Villains: Blood Pressure and Cholesterol
While blood sugar grabs all the headlines, controlling your blood pressure and cholesterol is just as vital for your foot health. High blood pressure puts constant, damaging strain on your artery walls, speeding up the damage that leads to poor circulation. High cholesterol adds to the problem by helping plaque build up in those arteries, narrowing them even more.
Managing the "ABCs of diabetes" is non-negotiable for protecting the fragile vascular network in your feet.
- A1c: Keeping your A1c in your target range is proof of good long-term glucose control.
- Blood Pressure: Work with your doctor to keep your blood pressure under control, which for most people with diabetes is typically below 130/80 mmHg.
- Cholesterol: Managing your LDL ("bad") cholesterol is key to keeping your arteries clear so blood can flow freely.
When you focus on your total diabetes management—glucose, blood pressure, and cholesterol—you're getting at the root causes of foot ulcers. It's this proactive, whole-body approach that offers the most powerful protection, helping to keep your feet healthy and ulcer-free for years to come.
The Importance of Professional Foot Examinations
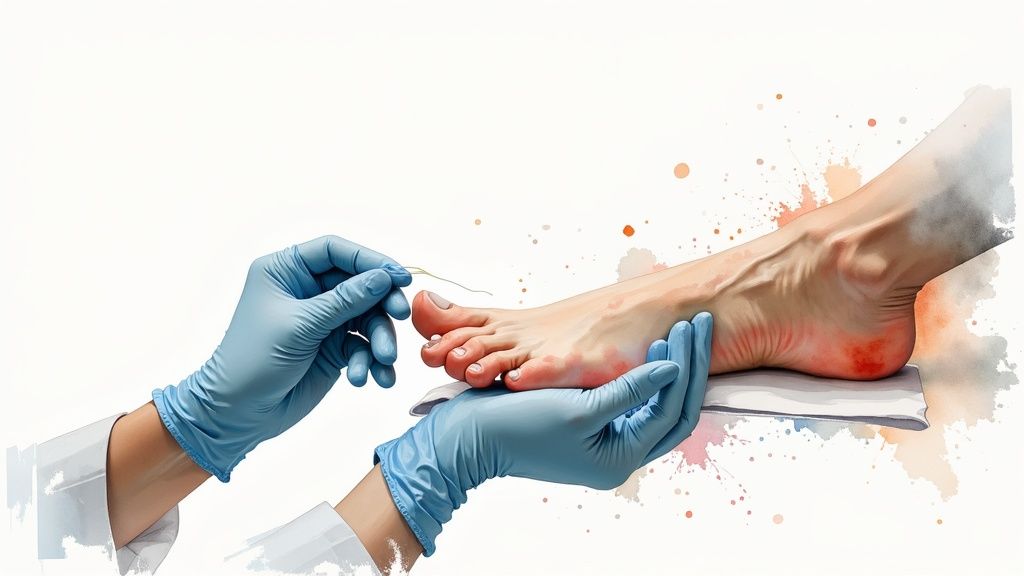
Your daily foot check is your first line of defense, but it can only go so far. Think of it this way: your daily routine is like a motion sensor on a security system. It's great for catching obvious problems. The professional exam, on the other hand, is the expert who reviews the footage and inspects the wiring, spotting subtle issues that could lead to a major breach.
Even the most diligent person can miss the tiny, almost imperceptible changes that signal the start of a serious problem. This is especially true if you have diabetic neuropathy, which can effectively silence the pain signals your body would normally send. A podiatrist has the tools and training to detect problems you simply cannot see or feel.
This is why an annual comprehensive foot exam isn't just a suggestion—it's absolutely essential. The data is clear: structured foot care programs built around annual exams and patient education can slash the incidence of diabetic foot ulcers by a staggering 30% to 60%. Even more critically, these programs have been shown to reduce major amputation rates by about 50% in high-risk individuals.
What Happens During a Comprehensive Foot Exam
A professional exam is much more than just a quick look at your feet. It's a detailed assessment designed to pinpoint your specific risk level for developing an ulcer. Your podiatrist will run a series of tests to check three critical areas of foot health: neurological, vascular, and dermatological.
Here’s a breakdown of what you can expect:
- Sensory Testing: Your podiatrist will likely use a monofilament—a soft, flexible nylon fiber—to test for any loss of protective sensation. They’ll touch various points on your feet and ask if you can feel it. It’s a simple, painless test, but it’s the gold standard for identifying neuropathy.
- Vascular Assessment: They will check the pulses in your feet (the dorsalis pedis and posterior tibial pulses) to evaluate your blood flow. They might also check your capillary refill time, which shows how quickly blood returns to your skin after pressure is applied.
- Skin and Structural Evaluation: The doctor will carefully inspect your skin for any calluses, blisters, or "hot spots" that indicate excess pressure. They’ll also assess your foot's structure, looking for deformities like bunions or hammertoes that could create friction points inside your shoes.
To help you feel more prepared for your next appointment, here's a look at what a thorough exam covers.
Your Annual Diabetic Foot Exam Checklist
This table breaks down the key assessments performed during a professional foot exam. Use it to understand what to expect and what questions to ask your provider.
| Assessment Component | What It Checks For | Why It Matters for Prevention |
|---|---|---|
| Monofilament Test | Loss of protective sensation (neuropathy). | Detects nerve damage that could prevent you from feeling a small injury. |
| Vascular Pulse Check | Strength and presence of blood flow to the feet. | Poor circulation slows healing and increases ulcer and infection risk. |
| Skin Integrity Inspection | Calluses, dryness, cracks, redness, or swelling. | Identifies pressure points or early signs of skin breakdown. |
| Foot Structure Evaluation | Deformities like bunions, hammertoes, or flat feet. | Pinpoints areas prone to rubbing and pressure inside footwear. |
| Toenail Assessment | Thickening, discoloration, or ingrown nails. | Prevents nail-related injuries that could become infected wounds. |
| Footwear Review | Proper fit, wear patterns, and appropriateness of shoes. | Ensures your shoes aren't contributing to pressure or friction. |
Remember, this exam is a crucial part of your preventative care strategy.
Partnering With Your Healthcare Team
Your relationship with your podiatrist and healthcare team should be a partnership. You are the expert on your own body, while they bring the clinical expertise. To make the most of this, you need to be an active participant in your care.
Come to your appointments prepared with questions. Don't be afraid to ask things that empower you to take better care of yourself.
Consider asking your doctor direct questions like, "Based on this exam, what is my personal risk level for developing an ulcer?" or "Are there any specific warning signs I should be watching for at home?" This approach ensures you leave with clear, personalized advice.
If the exam uncovers concerns like poor circulation or pressure spots, your provider may suggest more frequent check-ups or a referral to a specialist. If you already have a small wound or a suspicious area, getting expert care immediately is vital. In those situations, it's wise to book a consult with a wound care specialist for a dedicated treatment plan.
By combining your daily routine with an annual professional exam, you create a powerful, multi-layered strategy for keeping your feet safe and healthy.
Recognizing Red Flags and Acting Quickly
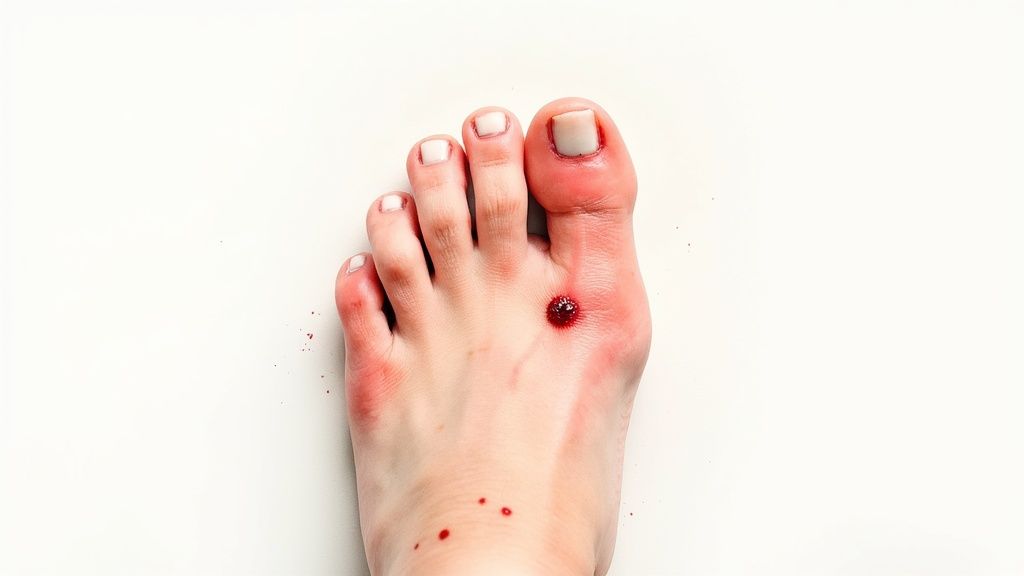
When it comes to diabetic foot care, hesitation is the enemy. Nerve damage, or neuropathy, often means your feet can't send the usual pain signals. A serious problem can develop without you feeling a thing, which makes your daily visual inspection absolutely critical—it's your only reliable alarm system.
Taking a "wait and see" approach is a gamble you just can't afford. A seemingly minor issue, like a small blister or a cut that isn't healing, can escalate into a severe infection in a matter of days. The goal is to spot these red flags early and get in touch with your doctor or podiatrist right away.
Immediate Action Warning Signs
If you notice any of these changes during your daily foot check, it’s time to pick up the phone. Don't try to treat these at home or hope they’ll get better on their own. These are clear signals that you need professional medical help immediately.
- Any Break in the Skin: This includes cuts, blisters, scrapes, or cracks, no matter how small. An open wound is a direct invitation for bacteria, and with diabetes, your body’s ability to fight infection and heal is often compromised.
- Drainage or Pus: Any fluid leaking from a sore is a major sign of infection, especially if it's cloudy, yellow, or greenish. You might also notice unexpected staining on your socks.
- Changes in Skin Color: Look for new redness, which points to inflammation or infection. Also, be alert for skin turning pale, blue, or black—this could indicate a severe lack of blood flow.
- Unusual Swelling: If one foot or part of your foot suddenly becomes swollen and puffy without a clear injury, it needs to be evaluated right away.
These signs are your body's way of shouting for help. Listening and acting quickly is a cornerstone of preventing a minor issue from becoming a limb-threatening emergency.
The Subtle but Serious Clues
Beyond the obvious, there are more subtle clues that something is wrong. These symptoms might not seem as alarming at first, but they are equally important red flags.
One of the most critical is a change in temperature. If one foot, or even just a specific spot, feels significantly warmer to the touch than the other, it can be an early sign of inflammation or a deep infection. This "hot spot" often shows up before any visible redness or swelling.
A foul odor coming from your foot or a sore that you can't explain is another major warning sign. This often points to an underlying infection with bacteria that produce gassy odors, and it requires urgent medical attention.
When to Contact a Wound Specialist
If you have a wound that isn't showing signs of improvement within a couple of days, or if you have any of the red flags we've discussed, don't hesitate. Your first step is contacting your healthcare provider. They can assess the situation and may refer you to a wound care specialist.
Advanced tools can help clinicians make faster, more informed decisions. For instance, understanding how a point-of-care wound imaging device detects bacteria shows how technology is supporting swift diagnosis and treatment. Early and expert intervention is the key to preventing a minor wound from turning into a major complication.
Common Questions on Preventing Diabetic Foot Ulcers
Even after you've learned the basics of diabetic foot care, real-world questions always pop up. Life with diabetes presents unique situations, and knowing how to handle them is a huge part of staying safe. This section dives into the most common questions we hear from patients, offering clear, straightforward answers to help you protect your feet.
Think of this as your go-to guide for those "what if" moments that can cause confusion. Getting these points straight will empower you to make smart, consistent choices for your foot health.
Is It Safe to Get a Pedicure If I Have Diabetes?
This is a question we get all the time, and the answer is a very cautious "maybe." A pedicure can feel wonderful, but it comes with real risks if you're not careful. The biggest dangers are infection from tools that haven't been properly sterilized and injuries from a technician being too aggressive.
If you still have good circulation and no nerve damage (neuropathy), you can consider it, but you have to be your own biggest advocate.
- Choose Your Salon Wisely: Find a reputable place that uses an autoclave for steam sterilization or opens a brand-new, single-use set of tools for every single client. Don't be afraid to ask to see their process.
- Speak Up Clearly: The moment you sit down, tell your nail technician that you have diabetes.
- Set Firm Boundaries: Instruct them not to cut your cuticles or use any sharp tools like razor blades to remove calluses. A gentle file is a much safer way to smooth rough spots. They should also not push back your nail folds aggressively.
But let's be clear: if you have significant neuropathy, poor circulation (peripheral artery disease), or any history of foot ulcers, you should avoid salon pedicures completely. In that case, your podiatrist is the only person who should be handling your nail and foot care.
What Kind of Socks Are Best for Diabetic Feet?
The right socks are just as critical as the right shoes. This is the material that's directly against your skin all day, so its features matter—a lot. Your goal is to find socks that protect your skin, pull moisture away, and never, ever restrict blood flow.
Here’s exactly what to look for:
- A Seamless Design: Seams are notorious for rubbing against the skin, causing friction that can lead to blisters and sores. A truly seamless sock gets rid of that risk.
- Moisture-Wicking Fabric: Steer clear of 100% cotton socks. They trap sweat right against your skin, creating a perfect environment for fungal infections and skin breakdown. Instead, opt for materials like wool, bamboo, or synthetic blends designed to wick moisture away.
- Non-Constricting Tops: That tight elastic band at the top of many socks can act like a tourniquet, impeding circulation. Look for non-binding or specifically labeled "diabetic" socks that stay up without squeezing your leg.
- Light Colors: This is a simple but effective trick. White or other light-colored socks make it much easier to spot any blood or drainage from a wound you might not be able to feel.
The best sock is one you forget you're even wearing. It cushions and protects without rubbing, constricting, or making your feet feel damp. It should feel like a soft, protective second skin.
Can I Go Barefoot at Home if My Floors Are Clean?
The answer you'll get from nearly every podiatrist is a firm, unwavering no. Even in the most spotless home, the risk of injury is just too high when you have diabetes, especially if neuropathy has set in. You simply can't feel a tiny splinter, a dropped pin, or the sharp corner of a coffee table you accidentally kick.
That tiny, unnoticed injury can quickly become a serious problem. A small cut you don't feel can go unnoticed for hours or even days. Always, always wear well-fitting slippers or supportive house shoes inside. This one simple habit creates a constant barrier between your feet and a world of unseen hazards.
How Does Smoking Affect My Risk for Foot Ulcers?
Smoking is one of the single most destructive habits for your foot health when you have diabetes. It wages a multi-front war on your circulatory system, drastically increasing your risk of getting an ulcer and crippling your body's ability to heal one.
Here’s how it happens: Nicotine causes your blood vessels to constrict and narrow, which immediately chokes off the supply of oxygen-rich blood that can reach your feet. At the same time, smoking accelerates atherosclerosis—the hardening and clogging of your arteries. This combination is a devastating one-two punch for the tiny, delicate blood vessels in your lower legs and feet.
Quitting smoking is one of the most powerful things you can do to learn how to prevent diabetic foot ulcers and protect yourself from amputation.
For more in-depth answers to other common concerns, you can find a wealth of information by exploring these frequently asked questions about wound care.
At Specialty Wound Care, we are committed to providing advanced, patient-centered solutions to heal complex wounds and prevent serious complications. If you or a loved one is struggling with a non-healing wound, learn how our expert team can help by visiting https://specialtywoundcare.com.









